One week after my first Substack post on Omicron there’s been a surge in new data. Here’s a quick timeline of the progress for what has been reported in just over 2 weeks since this new variant surfaced. To give you a sense of the remarkable velocity and collaborative capacity of the international science community effort, there have already been 10 lab neutralizations studies preprint published. They each require a lot of work culturing virus or pseudovirus and testing blood samples from people, either vaccinated or with prior Covid, against Omicron and other SARS-CoV-2 variants. All predicted the widely anticipated immune escape issues for Omicron with varying magnitude.
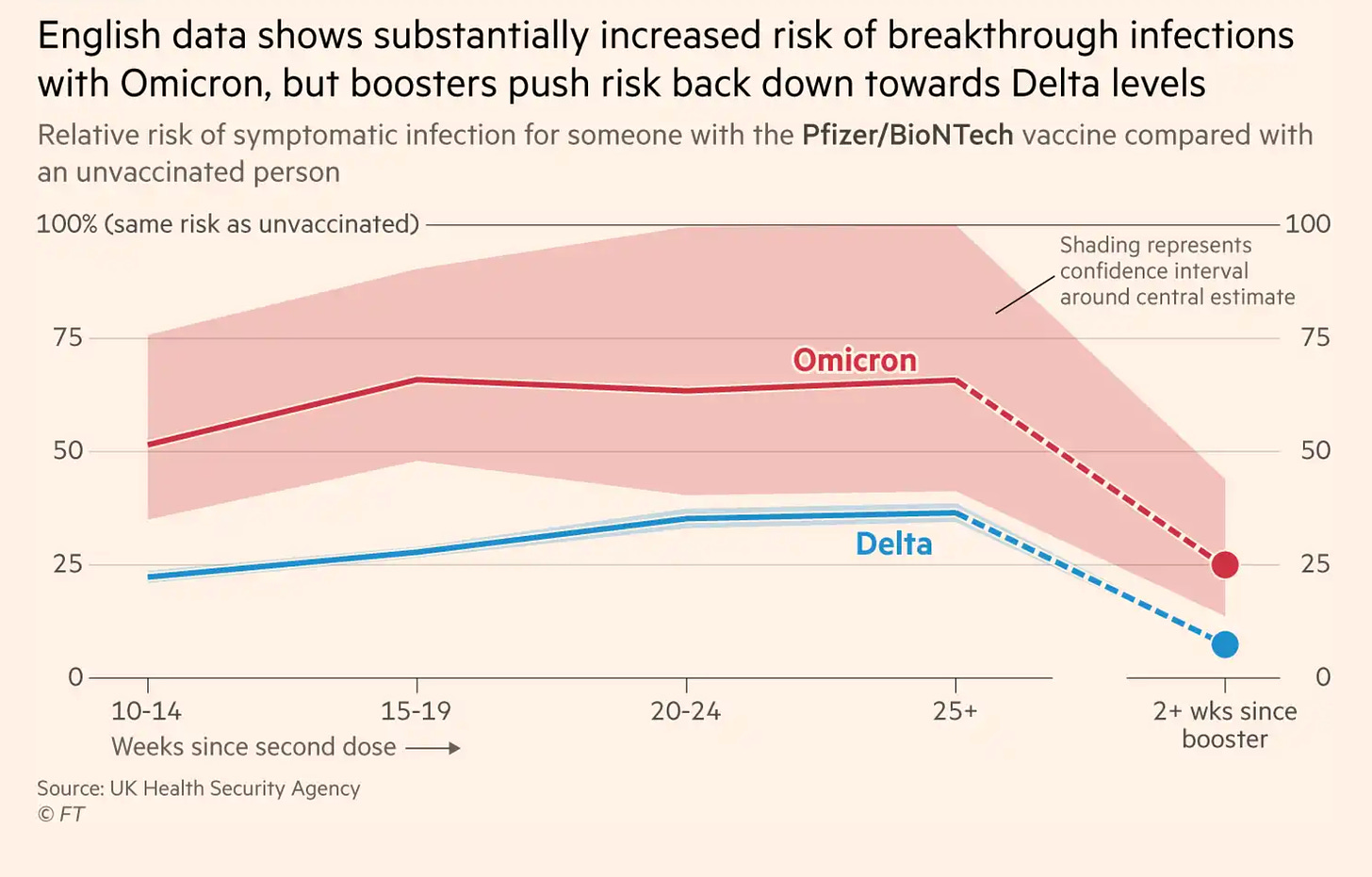
The big step beyond these lab studies was to get the first readout on vaccine effectiveness vs Omicron from the UK, summarized for Pfizer below vs symptomatic infection. For Delta, the prior >10 studies showed waning down to about 60% after 5 months, but restored from the booster to 95% by the large randomized (>10,000 participants) trial of 3 shots vs 2 shots + placebo, and multiple vaccine effectiveness studies from Israel and the UK. On the other hand, with Omicron, based on a limited number of UK cases the 2 dose protection dropped down to 34% and boosted up to 75%. That is a big decline from Delta for these point estimates, that would be potentially associated with about a 5-fold higher breakthrough infection rate after a booster. Added to this decline is the uncertainty as to how long it will last for either variant.
This graph below from the Financial Times shows the statistically difference with 95% confidence intervals before and after the third dose of Pfizer vaccine for Delta versus Omicron regarding protection against symptomatic infections. New data from South Africa indicate that the 2-dose Pfizer vaccine protection against severe Covid illness dropped from 93% for Delta to 70% for Omicron. There aren’t any data available yet for 3-dose vaccination vs severe Covid from Omicron.
These data points have come along with so much mixed news, as I’ve summarized in the Table below. From the same UK report we know the household contact transmission rate is about 3-fold increased compared with Delta. The rapid growth of Omicron is especially alarming, with a doubling rate between 2-3 days in multiple countries where it has been tracked (South Africa, UK, Germany, Denmark, Norway, Belgium US). This exponential rise could take us to levels of even 1 million cases per day in the United States, which previously would have been considered an unthinkable projection.
As I’ve written about for Omicron previously, we have the mitigation tools to defend against its transmission but have not been using them. California just re-instituted a state mask mandate which leverages that potential, a factor that had lapsed even as we are going through the second US Delta surge.
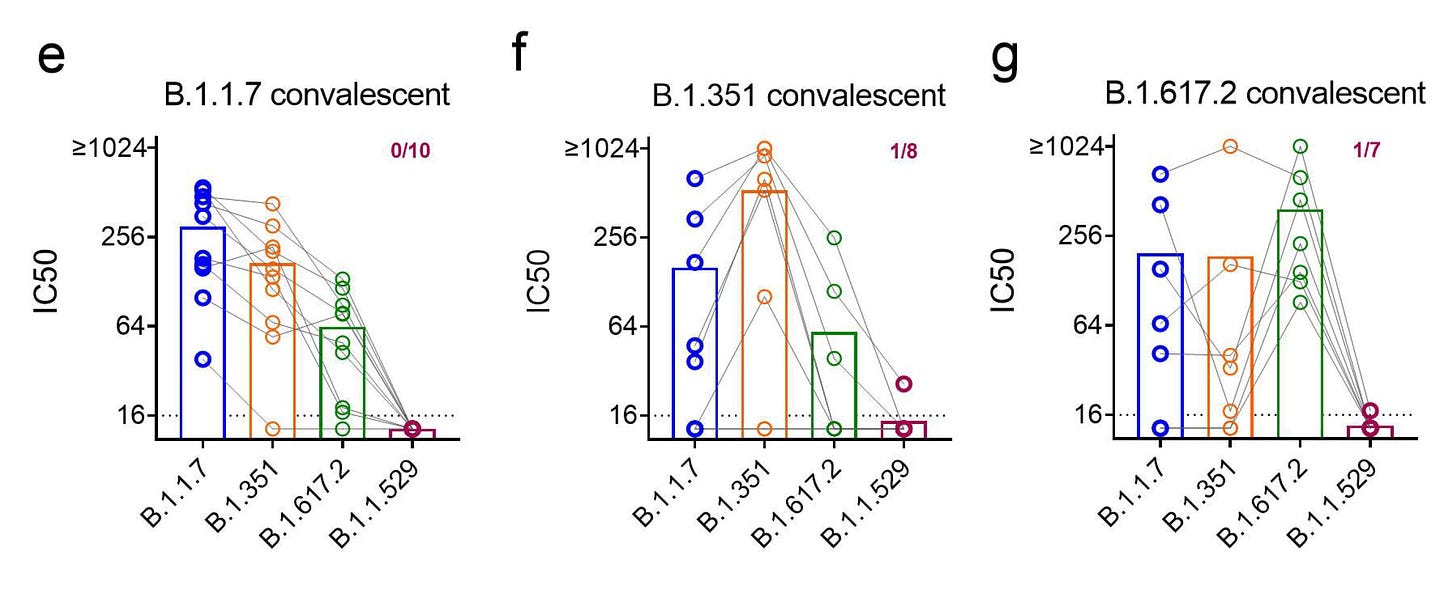
One of the issues that has been controversial is whether people with confirmed prior Covid need to get vaccinated. Overall, the data strongly support the benefit of at least 1 shot for generating “hybrid immunity,” that is the immune response to the full virus from an infection and the spike protein via the vaccine. But new data below show for Omicron there is very little neutralization antibody activity present in people who have had Covid infections from Alpha, Beta or Delta variants. Samples from people with infections from Alpha (B.1.1.7,) Beta (B.1.351), and Delta (B.1.617.2) showed minimal capacity to neutralize Omicron, and this was replicate by another study . The findings are in keeping with the high rate of reinfection for Omicron in people for prior Covid that was observed in South Africa (>2.4 X prior variants) and the UK (3-8 X Delta).
These 2 properties of Omicron—its high level of immune evasion and increased contagiousness—will compete with Delta and may well displace it as the global dominant strain. For example, in Denmark, the displacement of Omicron for Delta as dominant (>50% of cases) is expected to occur this week, and will inevitably be taking place in many other regions. Trevor Bedford has a very good thread on the potential of co-dominance of Delta and Omicron, because they have different features that may not allow one to fully dominate, Delta (relying on hits hyper-contagiousness) vs Omicron (combining considerable immune escape plus some increased contagiousness). No matter how this ultimately plays out, with the very high level of Delta circulating now in the United States, we will be dealing with both versions of the virus for some time ahead. Further, with the jump in Omicron’s immune evasion compared with Delta (and all prior variants), the potential for yet another new variant that even more effectively evades our immunity looms.
Now let me get to the critical issue of the mild severity that has been associated with Omicron to date. This is true, that where Omicron has been gaining steam, the proportion of hospitalizations is lower than expected, which is great. However, the main reason for this consistent observation is not the virus being less virulent, but the immunity wall that has been built in people throughout the 2 years of the pandemic. Beyond mitigation factors, there’s infection-acquired immunity and 3 lines of defense simplistically depicted below.
Prior Covid or 2 shots, as reviewed above, do not provide much defense against Omicron. The 3rd shot helps, but the effectiveness is considerably lower than what we have seen with Delta and prior to the waning that occurs over time. Our “last line of defense” is our T cell memory, which is induced by prior Covid and vaccinations. It isn’t rapid, doesn’t protect against the initial infection in our upper airway, but, on demand, kicks in to keep it there. This layer appears to be the main reason why Omicron appears mild—so many people have a T cell strong defense vs Covid pneumonia and other organ involvement. We can infer this from how well people in Southern Africa did with Omicron, with a relatively low per cent of hospitalizations despite low vaccination rates. There was, however, a high burden of prior infections there, and T cells are much less affected by different variants than our neutralizing antibody response. So we really won’t know whether there is something intrinsic to Omicron’s virulence until we see how it impacts people over age 60 who never had Covid or been vaccinated. If these people do not experience severe Covid, then we’ll be hunting for a mechanism to explain it. But right now we don’t need to invoke anything about Omicron, per se, being a milder virus. “It’s the immunity, stupid,” is my simplest, reductionist way to convey the reason for what we’ve seen so far.
But make no mistake, Omicron has the potential to induce an enormous number of infections worldwide and even if severe Covid is one-tenth that of Delta or preceding variants, in absolute numbers it could lead to a major toll of hospitalizations or deaths.
Similarly, we should not underestimate Omicron’s impact on Long Covid. The propagation of a large number of infections, even among vaccinated individuals, for whom there is expected to be some ill-defined lower risk and severity of Long Covid, is a lingering and serious concern. That’s why the promise of Paxlovid, a pill that has shown marked efficacy to stop the virus in its tracks, may play out to be important in reducing transmission and further lowering the risk of chronic Covid morbidity. More about that new layer of defense soon.
As Omicron’s rapid growth is paralleled by that of the science, we’ll know much more in upcoming days and I’ll try to summarize the ground truths and ideas here.