While the risk of severe, acute Covid that leads to hospitalization or death has decreased during the 3+ years of the pandemic, the primary concern has shifted to the chronic side—winding up with Long Covid. My colleagues and I reviewed Long Covid in-depth earlier this year, but there have been new reports that firm up evidence for 4 ways to reduce the likelihood of chronic sequelae from a Covid infection (or re-infection).
Novid
The first and only definitive way is to avoid Covid infections. As I previously reviewed, there are still approximately 10-15% of Americans who are likely Novids, never having been infected (potentially confirmed with negative anti-nucleocapsid antibodies), and that per cent will continue to decrease over time as the virus relentlessly finds new (and repeat) hosts.
A good quote from Mike Ryan of WHO from an excellent new piece on the ongoing threat
“You don’t want to get this disease once if you can avoid it, and you don’t want to get it four times for sure.”
Metformin
A randomized, placebo-controlled trial of metformin provides evidence for a second way, with a 42% reduction of Long Covid. A 2-week course of this very safe and inexpensive treatment was quite effective in a cohort age >30 and BMI >25, across multiple subgroups, as I have summarized. This is the only randomized trial to provide evidence for prevention vs Long Covid. Of course, we’d like to see the results replicated in another, larger trial of all comers, and fully understand the mechanism of the benefit, but given the magnitude of effect and the safety/cost issues, there appears to be little downside for use of metformin at this juncture.
In JAMA Internal Medicine, 2 new papers were published this week that firm up evidence for a 3rd and 4th means of preventing Long Covid.
Vaccination
A systematic review of 41 articles (distilled from 255 full-text papers reviewed and 5334 records), involving over 860,00 individuals, looked at risk factors for developing Long Covid, which included female sex (odds ratio 1.56), high BMI (OR 1.15), smoking (OR 1.1) and multiple comorbidities or hospitalization (OR 2.48). Vaccination was associated with an overall 43% reduction of Long Covid as shown below, with consistency of direction across all 4 studies assessing this relationship.
Paxlovid
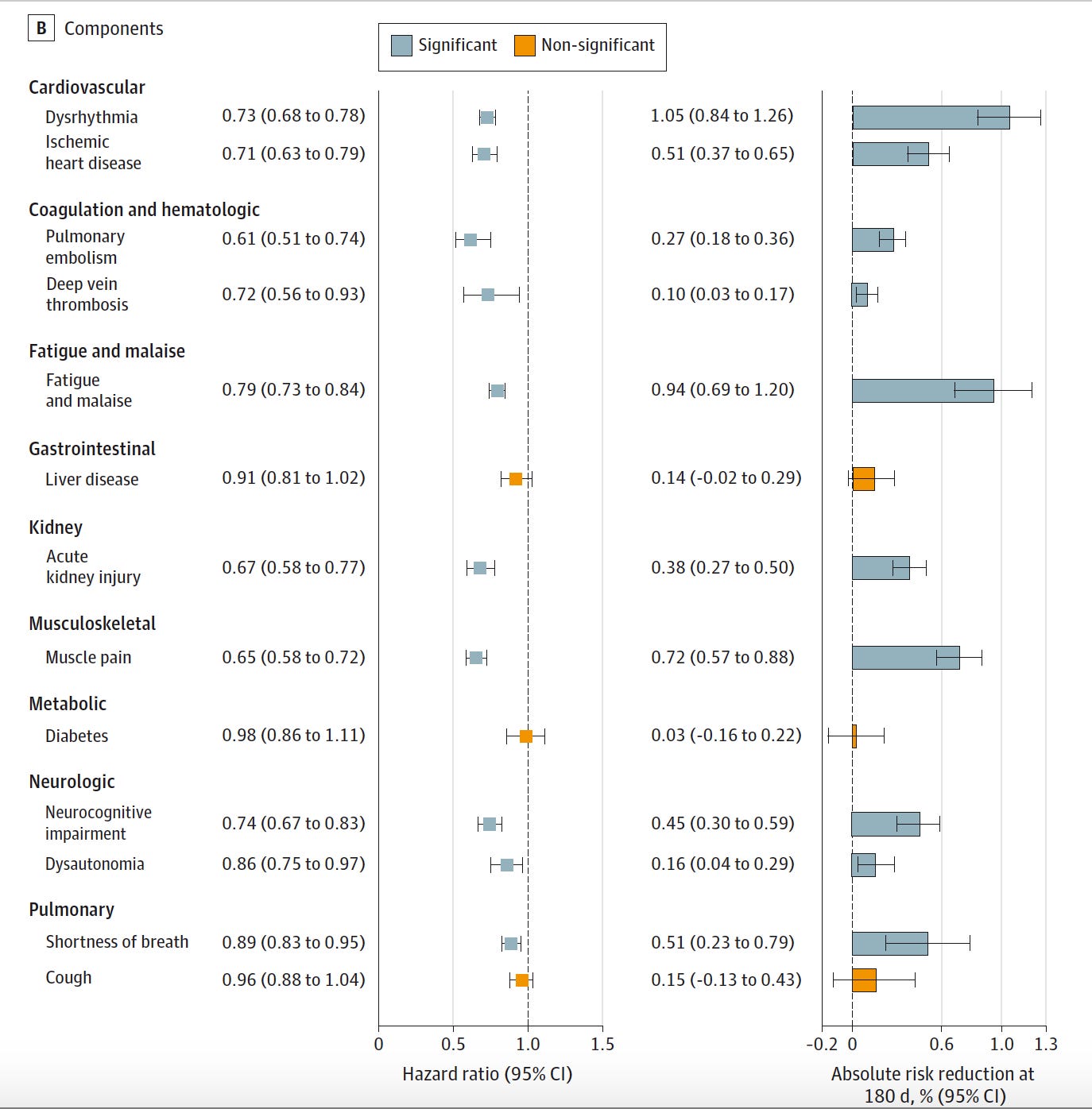
A preprint from the large Veterans Affairs data resource posted last November suggested that the use of Paxlovid was associated with a 26% reduction of Long Covid. Fortunately, the investigators have done considerably more in their final publication of these data, with nearly 4-fold more patients treated with Paxlovid and the follow-up extended from 90 days to 6 months. The very good news is that the 26% reduction has held up. For over 35,000 individuals treated within 5 days compared with ~246,000 controls there was a 26% reduction of Long Covid (Post-Covid Condition, PCC). Importantly, this benefit was across multiple organ system outcomes as shown below (no effect seen for reducing liver disease or diabetes).
The association of Long Covid protection was seen irrespective of vaccinated status
And consistently across different risk factor subgroups as seen below. Noteworthy, as I commented on for the preprint, is the population under study, mainly older White males. The lack of diversity and youth of the study population makes extrapolation of potential benefit across the board more difficult.
While the evidence supporting Paxlovid or vaccination protection vs Long Covid does not come from any randomized trials, both of these observational reports provide added support that was not previously available or aggregated, respectively. There was a recent Washington Post article about the potential of less Long Covid with Omicron compared with previous SARS-CoV-2 variants, but many confounders, such as infection and vaccination-induced immunity, make it difficult to assess.
OK, But What About Treatment?
It’s good that we now are seeing multiple ways to reduce the likelihood of developing Long Covid. But there has been no substantive progress for treating it. This week a small Paxlovid randomized study for treating people affected by Long Covid was announced and will start its enrollment of 100 participants next month, with 15 days of paxlovid or placebo and a full immunologic profile. A very large, randomized trial of Paxlovid should have been initiated a year ago, given the evidence of persistence of virus in reservoirs or remnants of virus, from multiple studies. Nonetheless, it is great that the Yale team, including Harlan Krumholz and Akiko Iwasaki, are now on it.
An article in today’s Rolling Stone (of all places) reviewed the potential of low-dose naltrexone and the fact it is getting frequently prescribed, with an excerpt below. In our Long Covid review, we highlighted naltrexone as a candidate drug for treatment but there is not yet adequate evidence to prove it is efficacious. A Canadian randomized trial of 160 participants is expected to provide data next year
That’s the up-to-date summary. We’re making progress for ways to reduce the chances of developing Long Covid, but far too little and slow on the treatment side. Hopefully, we’ll see much more in the way of testing the many candidate treatments in large, rigorous, randomized trials in the months ahead.
Thanks for reading, sharing and subscribing to Ground Truths.
As I’ve previously announced, if you decide to become a paid subscriber, I will donate all proceeds to Scripps Research.