Above is a brief video snippet from our conversation. Full videos of all Ground Truths podcasts can be seen on YouTube here. The audios are also available on Apple and Spotify.
Transcript with links to audio and external citations
Eric Topol (00:06):
Well, hello it's Eric Topol with Ground Truths, and I'm really delighted to welcome Dr. Rachael Bedard, who is a physician geriatrician in New York City, and is actually much more multidimensional, if you will. She's a writer. We're going to go over some of her recent writings. She's actually quite prolific. She writes in the New Yorker, New York Magazine, New York Times, New York Review of Books. If it has New York in front of it, she's probably writing there. She's a teacher. She works on human rights, civil rights, criminal justice in the prison system. She's just done so much that makes her truly unique. That's why I really wanted a chance to meet her and talk with her today. So welcome, Rachael.
Rachael Bedard (00:52):
Thank you, Dr. Topol. It's an honor to be here.
Eric Topol (00:55):
Well, please call me Eric and it's such a joy to have a chance to get acquainted with you as a person who is into so many different things and doing all of them so well. So maybe we'd start off with, because you're the first geriatrician we've had on this podcast.
Practicing Geriatrics and Internal Medicine
Eric Topol (01:16):
And it’s especially apropos now. I wanted maybe to talk about your practice, how you got into geriatrics, and then we'll talk about the piece you had earlier this summer on aging.
Rachael Bedard (01:32):
Sure. I went into medicine to do social justice work and I was always on a funny interdisciplinary track. I got into the Mount Sinai School of Medicine through what was then called the Humanities and Medicine program, which was an early acceptance program for people who were humanities focused undergrads, but wanted to go into medicine. So I always was doing a mix of politics and activist focused work, humanities and writing, that was always interested in being a doctor. And then I did my residency at the Cambridge Health Alliance, which is a social medicine program in Cambridge, Massachusetts, and my chief residency there.
(02:23):
I loved being an internist, but I especially loved taking care of complex illness and I especially loved taking care of complex illness in situations where the decision making, there was no sort of algorithmic decision-making, where you were doing incredibly sort of complex patient-centered shared decision making around how to come up with treatment plans, what the goals of care were. I liked taking care of patients where the whole family system was sort of part of the care team and part of the patient constellation. I loved running family meetings. I was incredibly lucky when I was senior resident and chief resident. I was very close with Andy Billings, who was one of the founders of palliative care and in the field, but also very much started a program at MGH and he had come to work at Cambridge Hospital in his sort of semi-retirement and we got close and he was a very influential figure for me. So all of those things conspired to make me want to go back to New York to go to the Sinai has an integrated geriatrics and palliative care fellowship where you do both fellowships simultaneously. So I came to do that and just really loved that work and loved that medicine so much. There was a second part to your question.
Eric Topol (03:52):
Is that where you practice geriatrics now?
Rachael Bedard (03:55):
No, now I have ever since finishing fellowship had very unusual practice settings for a geriatrician. So right out of fellowship, I went to work on Rikers Island and then New York City jail system, and I was the first jail based geriatrician in the country, which is a sort of uncomfortable distinction because people don't really like to think about there being a substantial geriatric population in jails. But there is, and I was incredibly lucky when I was finishing fellowship, there was a lot of energy around jail healthcare in New York City and I wrote the guy who was then the CMO and said, do you think you have an aging problem? And he said, I'm not sure, but if you want to come find out, we'll make you a job to come find out. And so, that was an incredible opportunity for someone right out of fellowship.
(04:55):
It meant stepping off the sort of academic track. But I went and worked in jail for six years and took care of older folks and people with serious illness in jail and then left Rikers in 2022. And now I work in a safety net clinic in Brooklyn that takes care of homeless people or people who have serious sort of housing instability. And that is attached to Woodhull Hospital, which is one of the public hospitals in New York City. And there I do a mix of regular internal medicine primary care, but I preferentially see the older folks who come through, which is a really interesting, painful, complicated patient population because I see a fair amount of cognitive impairment in folks who are living in the shelter system. And that's a really hard problem to address.
Frailty, The Aged, and Longevity
Eric Topol (05:54):
Well, there's a theme across your medical efforts. It seems to me that you look after the neglected folks, the prisoners, the old folks, the homeless people. I mean that's kind of you. It's pretty impressive. And there's not enough of people like you in the medical field. Now, no less do you do that, but of course you are a very impressive author, writer, and of many topics I want to get into with you, these are some recent essays you've written. The one that piqued my interest to start to understand who you were and kind of discover this body of work was the one that you wrote related to aging and President Biden. And that was in New York Times. And I do want to put in a quote because as you know very well, there's so much interest in longevity now.
Eric Topol (06:51):
Interrupting the aging process, and this one really stuck with me from that op-ed, “Time marches forward, bodies decline, and the growing expectation that we might all live in perfect health until our 100th birthdays reflects a culture that overprizes longevity to the point of delusion.” So maybe if you could tell us, that was a rich piece, you got into frailty, you related it to the issues that were surrounding President Biden who at that time had not withdrawn from the race. But what were you thinking and what are your thoughts about the ability to change the aging process?
Rachael Bedard (07:36):
I am very interested in, I mean, I'm incredibly interested in the science of it. And so, I guess I think that there are a few things.
(07:49):
One thing is that the framework that, the part that gives me pause the most is this framework that anything less than perfect health is not a life worth living. So if you're going to have a long life, life should not just be long and sort of healthy in relative terms to your age cohort, but healthy that when you're 80 you should feel like you have the health of a 45-year-old is my understanding of the culture of longevity science. And while I understand why that's aspirational and everybody worry about my body's decline, I think it's a really problematic thing to say that sick bodies are bodies that have disability or people who have cognitive difference are somehow leading lesser lives or lives that are not meaningful or not worth living. I think it's a very, very slippery slope. It puts you in a place where it sort of comes up against another trend or another emerging cultural trend, which is really thinking a lot about physician-assisted suicide and end of life choices.
(09:04):
And that in some ways that conversation can also be very focused on this idea that there's just no way that it's worth living if you're sick. And that's just not true, I think, and that's not been true for many, many, many of my patients, some of whom have lived with enormous disability and incredible burden of illness, people who are chronically seriously ill and are still leading lives that for them and for the people who love them are filled with meaning. So that's my concern about the longevity stuff. I'm interested in the science around the longevity stuff for sure. I'm interested in, I think we're living in this really interesting moment where there's so much happening across so many of the chronic disease fields where the things that I think have been leading to body decay over the last several decades for the majority of the population, we're sort of seeing a lot of breakthroughs in multiple fronts all at once. And that's really exciting. I mean, that's really exciting. And so, certainly if it's possible to make it to 100 in wonderful health, that's what I'd wish for all of us. But to hold it up as the standard that we have to achieve, I think is both unrealistic and a little myopic.
Eric Topol (10:28):
Yeah. Well, I certainly agreed with that and I think that that particular essay resonated so well and you really got into frailty and the idea about how it can be potentially prevented or markedly delayed. And I think before we move on to one of those breakthroughs that you were alluding to, any comments about the inevitability of frailty in people who are older, who at some point start to get the dwindles, if you will, what do you have to say about that?
Rachael Bedard (11:11):
Well, from a clinical standpoint, I guess the caveat versus that not everybody becomes frail and dwindles exactly. Some people are in really strong health up until sort of their final years of life or year of life and then something happens, they dwindle quickly and that's how they die. Or some people die of acute events, but the vast majority of us are going to become more frail in our final decades than we are in our middle decades. And that is the normal sort of pattern of wear and tear on the body. And it is an extraordinary framework, I think frailty because the idea of this sort of syndrome of things where it's really not a disease framework, it is a syndrome framework and it's a framework that says many, many small injuries or stressors add up to create a lot of stress and change in a body and trauma for our body. And once you are sort of past a tipping point of an amount of stress, it's very hard to undo those things because you are not sort of addressing one pathologic process. You're addressing, you're trying to mitigate many processes all at once.
(12:31):
When I wrote that piece, it was inspired by the conversation surrounding President Biden's health. And I was particularly struck by, there was a huge amount of clinical speculation about what was going on with him, right? I'm sure you remember there were people, there was all of this talk about whether he had Parkinson's and what his cognitive status was. And it felt to me like there was an opportunity to do some public education around the idea that you need not have one single sort of smoking gun illness to explain decline. What happens to most of us is that we're going to decline in many small ways sort of simultaneously, and it's going to impact function when it tips over a little bit. And that pattern of decline is not going to be steady day over day worsening. It's going to be up and down. And if you slept better the night before, you might have a better day the next day. And if you slept badly, you might have a worse day. And without knowing anything specific about his clinical situation, it felt like a framework that could explain so much of what we were seeing in public. And it was important also, I think to say that nothing was necessarily being hidden from anybody and that this is the kind of thing that, this has accumulated stress over time that then presents suddenly all at once after having been submerged.
Eric Topol (14:01):
Yeah, you reviewed that so well about the wear and tear and everything related to that. And before I move on to the second topic, I want to just circle back to something you alluded to, which is when Peter Attia wrote about this medicine 3.0 and how you would be compressed and you'd have no comorbidities, you'd have no other illnesses and just fall off the cliff. As a geriatrician, do you think that that is even conceivable?
Rachael Bedard (14:35):
No. Do you think it is?
Eric Topol (14:37):
No, but I just wanted to check the reality. I did challenge on an earlier podcast and he came up with his pat answer. But no, there's no evidence of that, that maybe you can delay if there ever was a way to do that. But I think there's this kind of natural phenomena that you just described, and I'll refer people also to that excellent piece that you get into it more.
Rachael Bedard (15:06):
Peter Attia, I mean, he is certainly the sort of standard bearer in my mind of that movement and that science or that framework of thinking about science. And there's stuff in there that's really valuable. The idea of thinking about lifestyle in your middle decades is having meaningful impact on how you will age, what your final years will look like. That seems intuitively true, I think. And so, thinking about his emphasis on exercise, I mean, his emphasis on exercise is particularly intense and not super achievable for the average person, but the idea that you should sort of be thinking about keeping your body strong because it will decline eventually. And so, you want to do that from a higher peak. That makes a lot of sense to me. The idea that where we sort of draw pathologic disease cutoffs is obviously a little bit arbitrary. And so, wanting to think about optimizing pre-disease states and doing prevention, that's obviously, I think pretty appealing and interesting. It's just really in an evidence free zone.
Ozempic for the Indigent
Eric Topol (16:18):
Yeah, that's what I confronted him with, of course, he had a different perspective, but you summed that up really well. Now let's switch to a piece you had in New York magazine. It was entitled, What If Ozempic Is Just a Good Thing? And the reason, of course, this ties into the first thing we're discussing. There's even talk now, the whole GLP-1 family of drugs with the dual triple receptors, pills to come that we're going to be able to interrupt a path towards Alzheimer's and Parkinson's. Obviously you've already seen impact in heart disease, liver disease, kidney disease way before that, diabetes and obesity. So what are your thoughts? Because you wrote a very interesting, you provided a very interesting perspective when you wrote that one.
Rachael Bedard (17:11):
So that piece I wrote because I have this unbelievably privileged, interesting clinical practice. In New York City, there is public health insurance basically available to anybody here, including folks who are undocumented. And the public hospital system has pharmacies that are outpatient pharmacies that have, and New York Medicaid is very generous and they arranged through some kind of brilliant negotiating. I don't quite know how to make Ozempic to make semaglutide available to people who met criteria which meant diabetes plus obesity, but that we could prescribe it even for our very, very poor patients and that they would be able to get it reliably, that we would have it in stock. And I don't know how many other practices in the country are able to reliably provide GLP-1s to marginalized folks like that. I think it feels like a really rare opportunity and a very distinct perspective.
(18:23):
And it has just been the most amazing thing, I think to have this class of drugs come along that, as you say, addresses so many problems all at once with at least in my prescribing experience, a relatively mild tolerable side effect profile. I have not had patients who have become incredibly sick with it. And for folks where making that kind of impact on their chronic illness is so critical to not just their longevity, but their disease status interacts so much with their social burden. And so, it's a very meaningful intervention I think around poverty actually.
(19:17):
I really feel that almost all of the popular press about it has focused very much on use amongst the wealthy and who's getting it off label and how are they getting it and which celebrities are taking it, and what are the implications for eating and diet culture and for people who have eating disorders. And that's a set of questions that's obviously sort of interesting, but it's really interesting in a very rarefied space. There's an unbelievable diabetes epidemic in this country, and the majority of people who have diabetes are not the people who are getting written about over and over again in those pieces. It's the patients that I take care of, and those people are at risk of ending up on dialysis or getting amputations. And so, having a tool this effective is really miraculous feeling to me.
Eric Topol (20:10):
Well, it really gives me some hope because I don't know any program like that one, which is the people who need it the most. It's getting provided for them. And we have been talking about a drug that costs a thousand dollars a month. It may get down to $500 a month, but that's still a huge cost. And of course, there's not much governmental coverage at this point. There might be some more for Medicare, Medicaid, whatever in the future, but it's really the original criteria of diabetes, and it took almost 20 years to get to where we are right now. So what's so refreshing here is to know that there's at least one program that is helping to bridge the inequities and to not make it as was projected, which was, as you say, for celebrities and wealthy people more exclusively, so that's great. And we still don't know about the diverse breadth of these effects, but as you well know, there's trials in Alzheimer's. I spoke to Steve Horvath recently on the podcast and he talked about how it's reset the epigenetic clock, GLP-1.
Rachael Bedard (21:24):
Does he think so?
Eric Topol (21:26):
Whoa. Yeah, there was evidence that was just presented about that. I said, well, if that does correspond to aging, the thing that we spoke about first, that would be very exciting.
Rachael Bedard (21:37):
It’s so wild. I mean, it's so exciting. It's so exciting to me on so many levels. And one of them is it's just exploding my mental model of disease pathogenesis, and it's making me think, oh my goodness, I have zero idea actually how metabolism and the brain and sort of cardiovascular disease, all of those things are obviously, what is happening in the interplay between all of those different systems. It's really so much more complicated and so much more interdependent than I understood it to be. I am really optimistic about the Alzheimer's trial. I am excited for those results, and I think we're going to keep seeing that it prevents different types of tumors.
Eric Topol (22:33):
Yeah, no, and that's been shown at least certainly in obese people, that there’s cancers that gets way reduced, but we never had a potent anti-inflammatory that works at the brain and systemically like this before anyone loses the weight, you already see evidence.
Long Covid and ME/CFS
(22:50):
It is pretty striking. Now, this goes back to the theme that was introduced earlier about looking after people who are neglected, who aren't respected or generally cared for. And I wanted to now get into Long Covid and the piece you wrote in the New Yorker about listening to patients, called “what would it mean for scientists to listen to patients?” And maybe you can talk about myalgic encephalitis/chronic fatigue (ME/CFS), and of course Long Covid because that's the one that is so pervasive right now as to the fact that these people don't get respect from physicians. They don't want to listen to their ailments. There's no blood tests, so there's no way to objectively make a diagnosis supposedly. And they're basically often dismissed, or their suffering is discounted. Maybe you can tell us again what you wrote about earlier this year and any updated thoughts.
Rachael Bedard (24:01):
Have you had my friend Harlan Krumholz on the show to talk about the LISTEN study?
Eric Topol (24:04):
Not yet. I know Harlan very well. Yes.
Eric Topol (24:11):
I know Akiko Iwasaki very well too. They’re very, very close.
Rachael Bedard (24:14):
So, Akiko Iwasaki and Harlan Krumholz at Yale have been running this research effort called the LISTEN study. And I first learned about it sometime in maybe late 2021. And I had been really interested in the emerging discourse around chronic illness in Long Covid in the 2021. So when we were past the most acute phase of the pandemic, and we were seeing this long tail of sequelae in patients, and the conversation had really shifted to one that was about sort of trying to define this new syndrome, trying to understand it, trying to figure out how you could diagnose it, what were we seeing sort of emerge, how are we going to draw boxes around it? And I was so interested in the way that this syndrome was really patient created. It came out of patients identifying their own symptoms and then banning together much, much faster than any kind of institutional science can ever work, getting into message boards together or whatever, and doing their own survey work and then coming up with their own descriptive techniques about what they were experiencing.
(25:44):
And then beyond that, looking into the literature and thinking about the treatments that they wanted to try for themselves. Patients were sort of at the forefront of every step of recognizing, defining, describing this illness presentation and then thinking about what they wanted to be able to do for themselves to address it. And that was really interesting to me. That was incredibly interesting to me. And it was also really interesting because by, I don't know exactly when 2021 or 2022, it was already a really tense landscape where it felt like there were real factions of folks who were in conflict about what was real and what wasn't real, how things ought to be studied, who ought to be studying them, what would count as evidence in this realm. And all of those questions were just really interesting to me. And the LISTEN study was approaching them in this really thoughtful way, which was Harlan and Akiko sort of partnering really closely with patients who enrolled.
(26:57):
And it's a decentralized study and people could enroll from all over the world. There's a portion of patients who do have their blood work evaluated, but you can also just complete surveys and have that data count towards, and those folks would be from anywhere in the world. Harlan did this amazing, amazing work to figure out how to collect blood samples from all over the country that would be drawn at home for people. So they were doing this decentralized study where people from their homes, from within the sort of circumstances of their lives around their chronic illness could participate, which that was really amazing to me. And then they were partnering really thoughtfully with these patients just to figure out what questions they wanted to ask, how they wanted to ask them, and to try to capture a lot of multimodal data all at once.
(27:47):
Survey data, journaling so people could write about their own experience in a freeform journal. They were collecting blood samples, and they were holding these town halls. And the town halls were on a regular basis, Harlan and Akiko, and anybody who was in the study could come on, could log onto a Zoom or whatever, and Harlan and Akiko and their research staff would talk about how things were going, what they were working on, what questions they had, what the roadblocks were, and then they would answer questions from their participants as the study was ongoing. And I didn't think that I had ever heard of something quite like that before. Have you ever heard of anything?
Eric Topol (28:32):
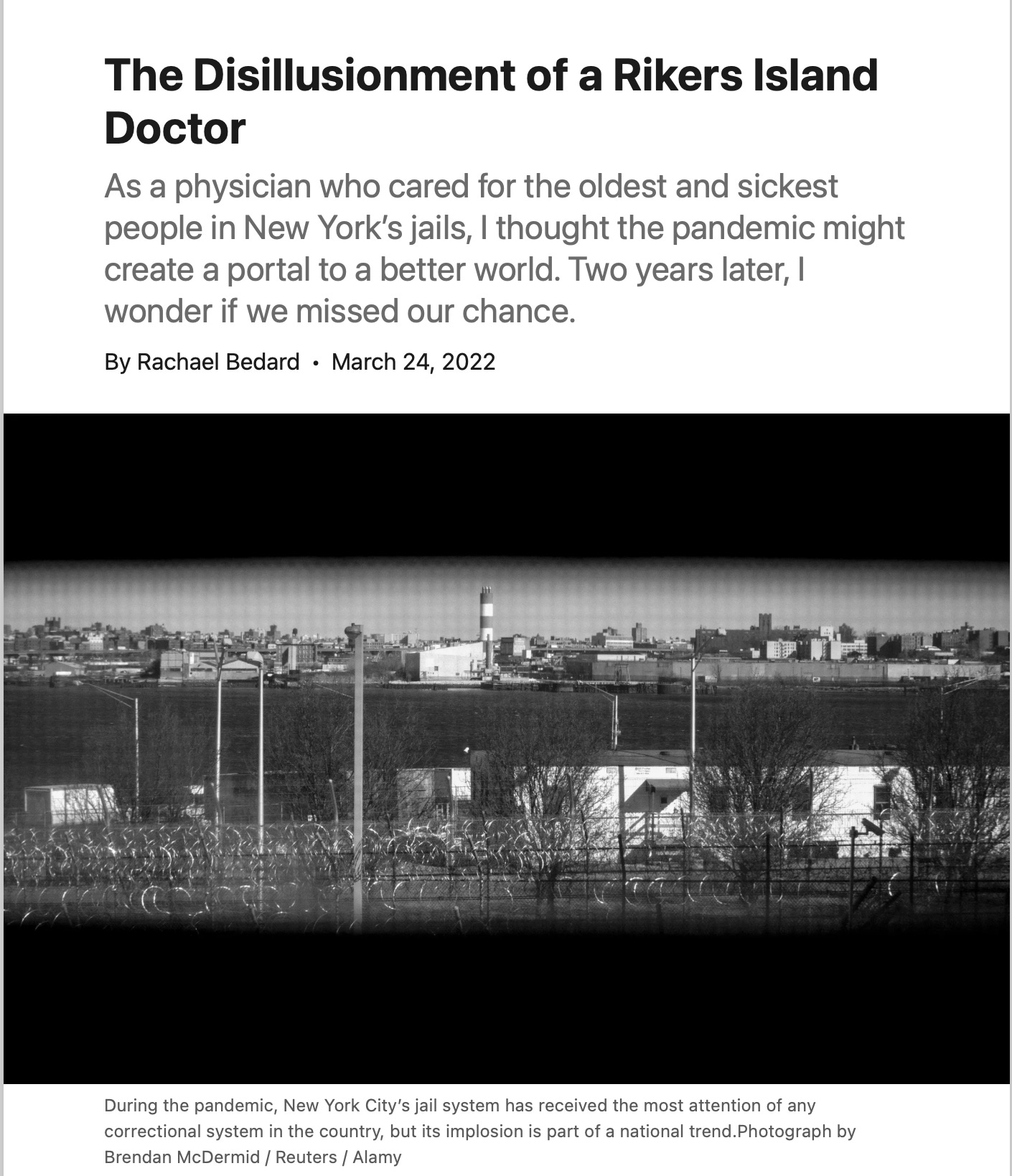
No. I mean, I think this is important to underscore, this was the first condition that was ever patient led, patient named, and basically the whole path was laid by the patient. So yes, and everything you summarize is so well as to the progress that's been made. Certainly, Harlan and Akiko are some of the people that have really helped lead the way to do this properly as opposed to, unfortunately one and a half billion dollars that have been put to the NIH for the RECOVER efforts that haven't yet led to even a significant clinical trial, no less a validated treatment. But I did think it was great that you spotlighted that just because again, it's thematic. And that gets me to the fourth dimension, which is you're the first prison doctor I've ever spoken to. And you also wrote a piece about that called, “the disillusionment of a Rikers Island Doctor” in the New Yorker, I think it was. And I wonder if you could tell us, firstly, now we're four years into Covid, you were for a good part of that at Rikers Island, I guess.
The Rikers Island Prison Doctor During Covid
Rachael Bedard (30:00):
I was, yeah.
Eric Topol (30:00):
Yeah. And what could be a more worrisome spot to be looking after people with Covid in a prison? So maybe you could just give us some insight about all that.
Rachael Bedard (30:17):
Yeah, it was really, I mean, it was the wildest time, certainly in my career probably that I'll ever have. In the end of February and beginning of March of 2020, it became very apparent to my colleagues and I that it was inevitable that this virus that was in Wuhan and in Italy was coming to the US. And jails are, we sort of jokingly described them as the worst cruise ships in the world. They are closed systems where everybody is eating, sleeping, going to the bathroom, everything on top of each other. There's an incredible amount of excess human contact in jails and prisons because people don't have freedom of movement and they don't get to do things for themselves. So every single, somebody brings you your mail, somebody brings you your meals, somebody brings you your medications. If you're going to move from point A to point B, an officer has to walk you there. So for a virus that was going to spread through what we initially thought was droplets and then found out was not just droplets but airborne, it was an unbelievably high-risk setting. It's also a setting where folks tend to be sicker than average for their age, that people bring in a lot of comorbidity to the setting.
(31:55):
And it's not a setting that does well under stress. I mean, jails and prisons are places that are sort of constitutionally violent, and they're not systems that adapt easily to emergency conditions. And the way that they do adapt tends to be through repressive measures, which tends to be violence producing rather than violence quelling. And so, it was just an incredibly scary situation. And in mid-March, Rikers Island, the island itself had the highest Covid prevalence of anywhere in the country because New York City was the epicenter, and Rikers was really the epicenter within New York. It was a wild, wild time. Our first seriously ill patient who ended up getting hospitalized. That was at that time when people were, we really didn't understand very much about what Covid looked like. And there was this guy sitting on the floor and he said, I don't know. I can't really get up.
(32:59):
I don't feel well. And he had an O2 stat of 75 or something. He was just incredibly hypoxic. It's a very scary setting for that kind of thing, right? It's not a hospital, it's not a place where you can't deliver ICU level care in a place like that. So we were also really worried about the fact that we were going to be transferring all of these patients to the city hospitals, which creates a huge amount of extra burden on them because an incarcerated patient is not just the incarcerated patients, the officers who are with that person, and there are special rules around them. They have to be in special rooms and all of these things. So it was just a huge systems crisis and really painful. And we, early on, our system made a bunch of good guesses, and one of our good guesses was that we should just, or one of our good calls that I entirely credit my bosses with is that they understood that we should advocate really hard to get as many people out as we could get out. Because trying to just manage the population internally by moving people around was not going to be effective enough, that we really need to decant the setting.
(34:18):
And I had done all of this work, this compassionate release work, which is work to get people who are sick out of jail so that they can get treatment and potentially die in a free setting. And so, I was sort of involved in trying to architect getting folks who were sort of low enough security risks out of jail for this period of time because we thought that they would be safer, and 1500 people left Rikers in the matter of about six weeks.
Rachael Bedard (34:50):
Which was a wild, wild thing. And it was just a very crazy time.
Eric Topol (34:56):
Yeah. Well, the word compassion and you go together exceptionally well. I think if we learn about you through your writings, that really shines through and what you've devoted your care for people in these different domains. This is just a sampling of your writings, but I think it gives a good cross section. What makes you write about a particular thing? I mean, obviously the Rikers Island, you had personal experience, but why would you pick Ozempic or why would you pick other things? What stimulates you to go after a topic?
Rachael Bedard (35:42):
Sometimes a lot of what I write about relates to my personal practice experience in some way, either to geriatrics or death and dying or to the criminal justice system. I've written about people in death row. I've written about geriatrics and palliative care in sort of a bunch of different ways. I am interested in topics in medicine where things are not yet settled, and it feels very of the moment. I'm interested in what the discourse is around medicine and healthcare. And I am interested in places where I think the discourse, not just that I'm taking a side in that discourse, but where I think the framework of the discourse is a little bit wrong. And I certainly feel that way about the Ozempic discourse. And I felt that way about the discourse around President Biden, that we're having not just a conversation that I have a strong opinion about, but a conversation that I think is a little bit askew from the way that we ought to be thinking about it.
Eric Topol (36:53):
And what I love about each of these is that you bring all that in. You have many different points of view and objective support and they're balanced. They're not just trying to be persuasive about one thing. So, as far as I know, you're extraordinarily unique. I mean, we are all unique, but you are huge standard deviations, Rachael. You cover bases that are, as I mentioned, that are new to me in terms of certainly this podcast just going on for now a couple of years, that is covering a field of both geriatrics and having been on the corrections board and in prison, particularly at the most scary time ever to be working in prison as a physician. And I guess the other thing about you is this drive, this humanitarian theme. I take it you came from Canada.
Rachael Bedard (37:59):
I did.
Eric Topol (37:59):
You migrated to a country that has no universal health.
Rachael Bedard (38:03):
That's right.
Eric Topol (38:03):
Do you ever think about the fact that this is a pretty pathetic situation here?
Rachael Bedard (38:08):
I do. I do think about it all the time.
Eric Topol (38:10):
In our lifetime, we'll probably never see universal healthcare. And then if you just go a few miles up north, you pretty much have that.
Rachael Bedard (38:18):
Yeah, if you've lived in a place that has universal healthcare and you come here, it's really sort of hard to ever get your mind around. And it has been an absolute possessing obsession of my entire experience in the US. I've now been here for over 20 years and still think it is an unbelievably, especially I think if you work with marginalized patients and how much their lack of access compounds the difficulty of their lives and their inability to sort of stabilize and feel well and take care of themselves, it's really frustrating.
Advice for Bringing Humanities to Medicine in a Career
Eric Topol (39:14):
Yeah, yeah. Well, I guess my last question to you, is you have weaved together a career that brings humanities to medicine, that doesn't happen that often. What's your advice to some of the younger folks in healthcare as to how to pull that off? Because you were able to do it and it's not easy.
Rachael Bedard (39:39):
My main advice when people ask me about this, especially to students and to residents who are often the people who are asking is to write when you can or pursue your humanities interests, your critical interests, whatever it is that you're doing. Do it when you can, but trust that your career is long and that you have a lot of time. Because the thing that I would say is I didn't start publishing until I was in fellowship and before that I was busy because I was learning to become a doctor. And I think it's really important that my concern about being a doctor who's a hybrid, which so many of us are now. A doctor or something else is you really do want to be a good doctor. And becoming a good doctor is really hard. And it's okay if the thing that is preoccupying you for the first 10 years of your training is becoming a great clinician. I think that's a really, really important thing to do. And so, for my first 10 years for med school and residency and chief residency and fellowship, I would write privately on the side a fair amount, but not try to publish it, not polish that work, not be thinking in sort of a careerist way about how I was going to become a doctor writer because I was becoming a doctor. And that was really preoccupying.
(41:08):
And then later on, I both sort of had more time and mental space to work on writing. But also, I had the maturity, I think, of being a person who was comfortable in my clinical identity to have real ideas and insights about medicine that felt different and unique to me as opposed to, I barely understand what's going on around me and I'm trying to pull it together. And that's how I would've been if I had done it more, I think when I was younger. Some people are real prodigies and can do it right out the gate, but I wasn't like that.
Eric Topol (41:42):
No, no, I think that's really sound advice because that's kind of the whole foundation for everything else. Is there a book in the works or will there be one someday?
Rachael Bedard (41:53):
There may be one someday. There is not one now. I think about it all the time. And that same advice applies, which is I believe in being a late bloomer and taking your time and figuring out what it is you really want to do.
Eric Topol (42:10):
Yeah. Well, that's great. Have I missed anything? And obviously we only can get to know you in what, 40 minutes to some extent, but have I not touched on something that you want to bring up?
Rachael Bedard (42:23):
No, I don't think so. Thank you for this conversation. It's been lovely.
Eric Topol (42:28):
No, I really enjoyed it. I'll be following your career. It's extraordinary already and you've got decades ahead to make an impact and obviously thinking of all these patients that you look after and have in the past, it’s just extraordinary. So what a joy to talk with you, Rachael, and I hope we'll have a chance to do that again in the times ahead.
Rachael Bedard (42:51):
Me as well. Thank you so much for inviting me.
**********************************************
Thank you for listening, reading or watching!
The Ground Truths newsletters and podcasts are all free, open-access, without ads.
Please share this post/podcast with your friends and network if you found it informative!
Voluntary paid subscriptions all go to support Scripps Research. Many thanks for that—they greatly help fund our education and summer internship programs.
Thanks to my producer Jessica Nguyen and Sinjun Balabanoff for audio and video support at Scripps Research.
Note: you can select preferences to receive emails about newsletters, podcasts, or all I don’t want to bother you with an email for content that you’re not interested in.















Share this post