Professor Joseph Allen directs the Healthy Buildings Program at Harvard Chan School of Public Health. His expertise extends far beyond what makes buildings healthy. He has been a leading voice and advocate during the Covid pandemic for air quality and ventilation. He coined the term “Forever Chemicals” and has written extensively on this vital topic, no less other important exposures, which we covered In our wide-ranging conversation. You will see how remarkably articulate and passionate Prof Allen is about these issues, along with his optimism for solutions.
A video snippet of our conversation: buildings as the 1st line of defense vs respiratory pathogens. Full videos of all Ground Truths podcasts can be seen on YouTube here. The audios are also available on Apple and Spotify.
Transcript with External Links and Links to Audio
Eric Topol (00:00:06):
Well, hello. It's Eric Topol from Ground Truths and I am just delighted to have with me, Joseph Allen from the Harvard School of Public Health, where he directs the Healthy Buildings Program that he founded and does a whole lot more that we're going to get into. So welcome, Joe.
Joseph Allen (00:00:24):
Thanks. It's great to be here. I appreciate the invitation.
Joe Allen’s Background As A Detective
Eric Topol (00:00:28):
Well, you have been, as I've learned, rocking it for many years long before the pandemic. There's quite a background about you having been a son of a homicide detective, private eye agency, and then you were going to become an FBI agent. And the quote from that in the article that's the Air Investigator is truly a classic. Yeah, you have in there, “I guarantee I'm the only public health student ever to fail an FBI lie detector polygraph in the morning and start graduate school a few hours later.” That's amazing. That's amazing.
Joseph Allen (00:01:29):
All right. Well, you've done your deep research apparently. That's good. Yeah, my dad was a homicide detective and I was a private investigator. That's no longer my secret. It's out in the world. And I switched careers and it happened to be the day I took the polygraph at the FBI headquarters in Boston, was the same day I started graduate studies in public health.
Sick vs Healthy Buildings (Pre-Covid)
Eric Topol (00:01:53):
Well, you're still a detective and now you're a detective of everything that can hurt us or help us environmentally and my goodness, how grateful we are that you change your career path. I don't know anyone who's had more impact on buildings, on air, and we're going to get into chemicals as well. So if we go back a bit here, you wrote a book before the pandemic, talk about being prescient. It’s called Healthy Buildings: How Indoor Spaces Can Make You Sick - or Keep You Well with John Macomber, your co-author. What was it that gave you the insight to write a book before there was this thing called Covid?
Joseph Allen (00:02:41):
Yeah, well, thanks for making the connection too, my past career to current career. For many years, I thought there wasn't a connection, but I agree. There's actually a lot of similarities and I also am really appreciative. I am lucky I found the field of Public Health, it's clearly where I belong. I feel like I belong here. It's a place to make an impact that I want to make in my career. So yeah, the Healthy Buildings book, we started writing years before the pandemic and was largely motivated by, I think what you and others and other people in my field have known, is that buildings have an outsized impact on our health. Yet it's not something that comes to the forefront when you ask people about what matters for their health. Right, I often start presentations by asking people that, what constitutes healthy living? They'll say, I can't smoke, I have to eat well.
(00:03:30):
I have to exercise. Maybe they'll say, outdoor pollution’s bad for you. Very few people, if any, will say, well, the air I breathe inside my building matters a lot. And over the years I had started my public health career doing forensic investigations of sick buildings. People really can get sick in buildings. It can be anything from headaches and not being able to concentrate all the way to cancer clusters and people dying because of the building. And I've seen this in my career, and it was quite frustrating because I knew, we all knew how to design and operate buildings in a way that can actually keep people healthy. But I was frustrated like many in my field that it wasn't advancing. In other words, the science was there, but the practice wasn't changing. We were still doing things the wrong way around ventilation, materials we put in our building, and I would lecture over and over and give presentations and I decided I want to try something new.
(00:04:22):
I do peer-reviewed science. That's great. I write pieces like you for the public, and I thought we'd try a longer form piece in a book, and it's published by Harvard Press. John Macomber for those who know is a professor at Harvard Business School who's an expert in real estate finance. So he'd been talking about the economic benefits of healthier buildings and some hand waving as he describes around public health. I've been talking about the public health benefits and trying to wave an economic argument. We teamed up to kind of use both of our strengths to, I hope make a compelling case that buildings are good for health and they're also just good business. In other words, try to break down as many barriers as we can to adoption. And then the book was published right as Covid hit.
Indoor Air Quality and Cognition
Eric Topol (00:05:05):
Yeah. I mean, it's amazing. I know that typically you have to have a book almost a year ahead to have it in print. So you were way, way ahead of this virus. Now, I'm going to come back to it later, but there were two things beyond the book that are pretty striking about your work. One is that you did all these studies to show with people wearing sensors to show that when the levels of CO2 were high by sensors that their cognition indoors was suffering. Maybe you could just tell us a little bit about these sensors and why aren't we all wearing sensors so that we don't lose whatever cognitive power that we have?
Joseph Allen (00:05:56):
Well, yeah. First I think we will start having these air quality sensors. As you know, they're starting to become a lot more popular. But yeah, when I first joined the faculty full-time at Harvard, one of the first studies I conducted with my team was to look at how indoor air quality influences cognitive function. And we performed a double-blind study where we took people, office workers and put them in a typical office setting. And unbeknownst to them, we started changing the air they were breathing in really subtle ways during the day, so they didn't know what we were doing. At the end of the day, we administered an hour and a half long cognitive function battery, and like all studies, we control for things like caffeine intake, baseline cognitive performance, all the other factors we want to account for. And after controlling for those factors in a double-blind study, we see that indoor air quality, minor improvements to indoor air quality led to dramatic increases in cognitive function test scores across domains that people recognize as important for everyday life.
(00:06:59):
How do you seek out and utilize information? How do you make strategic decisions? How do you handle yourself during a crisis and importantly recover after that crisis? I don't mean the world's ending crisis. I mean something happens at work that's stressful. How do you handle that and how do you respond? Well, it turns out that amongst all the factors that influence how we respond there, indoor air quality matters a lot. We call that study the COGfx Study for cognitive function. We replicated it across the US, we replicated it across the world with office workers around the world, and again, always showing these links, the subtle impact of indoor air quality on cognitive function performance. Now, that also then starts to be the basis for some of the economic analysis we perform with my colleague at Harvard Business School. We say, well, look, if you perform this much better related to air quality, what would happen if we implemented this at scale in a business?
(00:07:51):
And we estimate that there are just massive economic gains to be had. On a per person basis, we found and published on this, that's about $6,000 to $7,000 per person per year benefit across a company. It could lead to 10% gains to the bottom line performance of the company. And again, I'm a public health professor. My goal is to improve people's health, but we add a lens, mental health, brain health is part of health, and we add the economic lens to say, look, this is good for a worker of productivity and the costs are downright trivial when you compare it against the benefits, even just including the cognitive function benefits, not even including the respiratory health benefit.
Eric Topol (00:08:33):
And I mean, it's so striking that you did these studies in a time before sensors were, and they still are not widely accepted, and it really helped prove, and when we start to fall asleep in a group session indoors, it may not just be because we didn't have enough sleep the night before, right.
Joseph Allen (00:08:56):
It's funny you say that. I talk about that too. It's like, do we actually need the study to tell us to quantify what we've all experienced these bad conference rooms, you get tired, you can't concentrate, you get sleepy while you're driving your car. Yeah, a whole bunch of other factors. Maybe the speaker's boring, but a key factor is clearly indoor air quality and things like good ventilation, the chemical load in the space are all contributing.
Eric Topol (00:09:20):
Yeah. No, it's pretty darn striking. Now we're going to get into the pandemic, and this of course is when your work finally crystallized that you've been working on this for years, and then finally your collaboration with some of the aerosol experts. It was a transdisciplinary synergy that was truly extraordinary. And when you were on 60 Minutes last October, you said, “Think about the public health gains we've made over the past hundred years. We've made improvements to water quality, outdoor air pollution, our food safety, we've made improvements to sanitation: absolute basics of public health. Where has indoor air been in that conversation?” You brought it to us. I mean, you led the Lancet Commission on this. You've done a White House Summit keynote. You had a lot of influence. Why did it take us to finally wake up to this issue that you've been working on for years?
Covid is Airborne, Denial
Joseph Allen (00:10:31):
Yeah. Well, I appreciate that, but I also liked what you started with. I mean, there's been a lot of us pulling on this, and I think one of the magical moments, if you could say that when the pandemic happened was that it forced these collaborations and forced a lot of us in our field to be a bit more vocal. And even that comment about the gains we made in public health, that comes from an article that we co-authored with 40 plus scientists around the world in science, trying to drive home the point that we've ignored one of the key factors that determines our health. We were all frustrated at the beginning of the pandemic. The first piece I wrote was January 2020, talking about healthy buildings as the first line of defense, airborne spread, ventilation, filtration. I could not get it published. I could not get it published.
(00:11:20):
So I moved it to an international paper. I wrote it in the Financial Times in early February, but it wasn't until mid-March that the Times took my piece on this airborne spread buildings ventilation. At the same time, we know people like Linsey Marr, Rich Corsi, many others, Shelly Miller out there publishing, doing the fundamental research, all trying to elevate, and I think we started to find each other and say, hey, someone's trying to hit the medical journals. We're not landing there. I'm trying to hit the Times, and we’re not landing there. We're trying to get the reporters to pay attention. It's not landing there. Let's team up. Let's write these joint pieces. And I think what happened was you saw the benefit of the collective effort and interdisciplinary expertise, right? We could all start to come together, start instead of having these separate voices, a little bit of a unified voice despite important scientific minor disagreements, but start to say, hey, we started elevate each other and said, this is really important. It's the missing component of the messaging in the early days of the pandemic, and to know how to defend yourself.
Eric Topol (00:12:20):
Well, I think a lot of people think the big miss, and I know you agree, was the lack of recognition of aerosol transmission instead of just liquid droplets. But what you brought to this was really your priors on the buildings themselves and the ventilation systems and air quality that was highly, I mean, critical to it isn't just the aerosol, it's obviously how buildings are set up. Now, there's an amazing piece of course that appeared in the summer of 2021 called the Air Investigator, which profiled you, and in it brings up several things that finally are, we're starting to get our act together. I mean, ultimately there was in May 2023 years later, the CDC says, we're going to do something about this. Can you tell us what was this very distinct new path that the CDC was at least saying? And also couple that with whatever action if or not action has been taken.
Joseph Allen (00:13:33):
Yeah. So there really was a monumental shift that took, it was years in development, but we finally won the argument, collectively that airborne spread was the dominant mode of transmission. Okay, we got that. Then the question is, well, what changes? Do we actually get guidance here? And that took a little bit longer. I give Rochelle Walensky a lot of credit when she came into the CDC, we talked with her about this. That's when you start to first see ventilation starts showing up and the guidance, including guidance for schools. So I think that was a big win, but still no one was willing to set an official target or standard around higher ventilation rates. So that's important. Early in the pandemic, some people started to hear a message, yes, ventilation is important. What's the obvious next question, well, how much, what do I need? So in the summer of 2020, actually Shelly Miller and I collaborated on this.
(00:14:23):
We published some guidance on ventilation targets for schools. We said four to six air changes per hour (ACH) and target that. Well, it wasn't until 2023, spring of 2023 that you mentioned that CDC published target ventilation rates, and they went with five air changes per hour, which is right where we were talking about in summer 2020. It's what the Lancet of COVID-19 Commission adopted, but it's momentous in this way. It's the first time in CDCs history they've ever published a ventilation rate target for health. Now, I know this seems slow at the time, and it was, but if we think about some of the permanent gains that will come out of the pandemic. Pandemic changes society and science and policy and practice this, we are never going back. Now buildings will be a first line of defense for respiratory pathogens going forward that can no longer be ignored. And now we have the published target by CDC. That's a big deal because it's not just a recognition, but there's actually something to shoot for out there. It's a target I happen to like, I think there are differences between different scientists, but ultimately we've lifted the floor and said, look, we actually have to raise ventilation rates and we have something to shoot for. The public needed that kind of guidance a lot earlier, of course, but it was a big deal that it happened. It’s just too bad it took until spring 2023.
Eric Topol (00:15:46):
Yeah, I certainly agree that it was momentous, but a year plus later, has there been any change as a result of this major proclamation, if you will?
Joseph Allen (00:15:59):
Well, I actually see a lot of change from a practitioner level, but I want to talk about it in two aspects. I see a lot of schools, universities, major companies that have made this shift. For example, in the 60 Minutes piece, I talk that I advised Amazon and globally they're measuring indoor air quality with real-time sensors in their buildings. I've worked with hundreds of school districts that have made improvements to indoor air quality. I know companies that have shifted their entire approach to how they design and operate their buildings. So it's happening. But what really needs to happen, Eric, if this movement is going to benefit everyone, is that these targets need to be codified. They need to go into building codes. It can't just be, oh, I've heard about this. So I made the decision. I have the resources and the money to make this improvement.
(00:16:44):
To create a healthy building or a healthy school, we need to be sure this gets built into our code. So it just becomes the way it's done. That is not happening. There are some efforts. There are some bills at the national level. Some states are trying to pass bills, and I have to say, this is why I'm optimistic. It feels very slow. I'm as frustrated as anybody. I wanted this done before the pandemic. As soon as the pandemic hit, we saw it. We knew what we needed to get done. It didn't happen. But if we think about the long arc here and the public health gains we're actually, it's remarkable to me that we actually have bills being introduced around indoor air quality that ASHRAE has set a new health focused target for the first time really in their history. CDC, first time. New buildings going up in New York City designed to these public health targets. That's really different. I've been in this field for 20 plus years. I've never seen anything like it. So the pace is still slow, but it really is happening. But it has to reach everybody, and the only way that's going to happen is really this gets into building codes and performance standards.
The Old Efficient Energy Buildings
Eric Topol (00:17:52):
Yeah. Well, I like your optimistic perspective. I do want to go back for a second, back decades ago there was this big impetus to make these energy efficient buildings and to just change the way the buildings were constructed so that there was no leak and it kind of set up this problem or exacerbated, didn't it?
Joseph Allen (00:18:19):
Yeah. I mean, I've written about this a lot. I write in the book our ventilation standards, they've been a colossal mistake. They have cost the public in terms of its health because in the seventies, we started to really tighten up our building envelopes and lower the ventilation rates. The standards were no longer focused on providing people with a healthy indoor space. As I write in the book, they were targeted towards minimally acceptable indoor air quality, bare minimums. By the way that science is unequivocal, is not protective of health, not protective against respiratory pathogens, doesn't promote good cognitive function, not good for allergies. These levels led to more illness in schools, more absences for teachers and students, an absolute disaster from a public health standpoint. We've been in this, what I call the sick building era since then. Buildings that just don't bring in enough clean outdoor air. And now you take this, you have a building stock for 40 years tighter and tighter and tighter bumps up against a novel virus that spread nearly entirely indoors. Is it any wonder we had, the disaster we had with COVID-19, we built these bills. They were designed intentionally with low ventilation and poor filtration.
Optimal Ventilation and Filtration
Eric Topol (00:19:41):
Yeah. Well, it's extraordinary because now we've got to get a reset and it's going to take a while to get this done. We'll talk a bit about cost of doing this or the investment, if you will, but let's just get some terms metrics straight because these are really important. You already mentioned ACH, the number of air changers per hour, where funny thing you recommended between four and six and the CDC came out with five. There's also the minimum efficiency reporting value (MERV). A lot of places, buildings have MERV 8, which is insufficient. We need MERV 13. Can you tell us about that?
Joseph Allen (00:20:23):
Yeah, sure. So I think when we think about how much, you have two ways to capture these respiratory particles, right? Or get rid of them. One is you dilute them out of the building or you capture them on filters. You can inactivate them through UV and otherwise. But let's just stay on the ventilation and filtration side of this. So the air changing per hour is talking about how often the air is change inside. It's an easy metric. There are some strengths to it, there's some weaknesses, but it's intuitive and I'll you some numbers so you can make sense of this. We recommended four to six air changes per hour. Typical home in the US has half an air change per hour. Typical school designed to three air changes per hour, but they operate usually at one and a half. So we tried to raise this up to four, five, or six or even higher. On the filtration side, you mentioned MERV, right? That's just a rating system for filters, and you can think about it this way. Most of the filters that are in a building are cheap MERV 8 filters, I tend to think of them as filters that protect the equipment. A MERV 13 filter may capture 80 or 90% of particles. That's a filter designed to protect people. The difference in price between a MERV 8 and a MERV 13 is a couple of bucks.
(00:21:30):
And a lot of the pushback we got early in the pandemic, some people said, well, look, there's a greater resistance from the better filter. My fan can't handle it. My HVAC system can't handle it. That was nonsense. You have low pressure drop MERV 13 filters. In other words, there really wasn't a barrier. It was a couple extra bucks for a filter that went from a MERV 8 might capture 20 or 30% to a filter, MERV 13 that captures 80 or 90% with very little, if any impact on energy or mechanical system performance. Absolute no-brainer. We should have been doing this for decades because it also protects against outdoor air pollution and other particles we generate indoors. So that was a no-brainer. So you combine both those ventilation filtration, some of these targets are out there in terms of air change per hour. You can combine the metric if we want to get technical to talk about it, but basically you're trying to create an overall amount of clean air. Either you bring in fresh outdoor air or you filter that air. It really is pretty straightforward, but we just didn't have some of these targets set and the standards we're calling for these minimum acceptable levels, which we're not protective of health.
Eric Topol (00:22:37):
So another way to get better air quality are these portable air cleaners, and you actually just wrote about that with your colleagues in the Royal Society of Chemistry, not a journal that I typically read, but this was an important article. Can you give us, these are not very expensive ways to augment air quality. Can you tell us about these PACs ?
Joseph Allen (00:23:06):
These portable air cleaners (PACs), so the same logic applies if people say, well, I can't upgrade my system. That's not a problem for very low cost, you could have, these devices are essentially a fan and a filter, and the amount of clean air you get depends on how strong the fan is and how good the filter is. Really pretty simple stuff here, and you can put one of these in a room if it's sized right. My Harvard team has built tools to help people size this. If you're not quite sure how to do it, we have a technical explainer. Really, if you size it right, you can get that four, five or six air changes per hour, very cheap and very quickly. So this was a tool I thought would be very valuable. Rich Corsi and I wrote about this all through the summer of 2020 to talk about, hey, a stop gap measure.
(00:23:50):
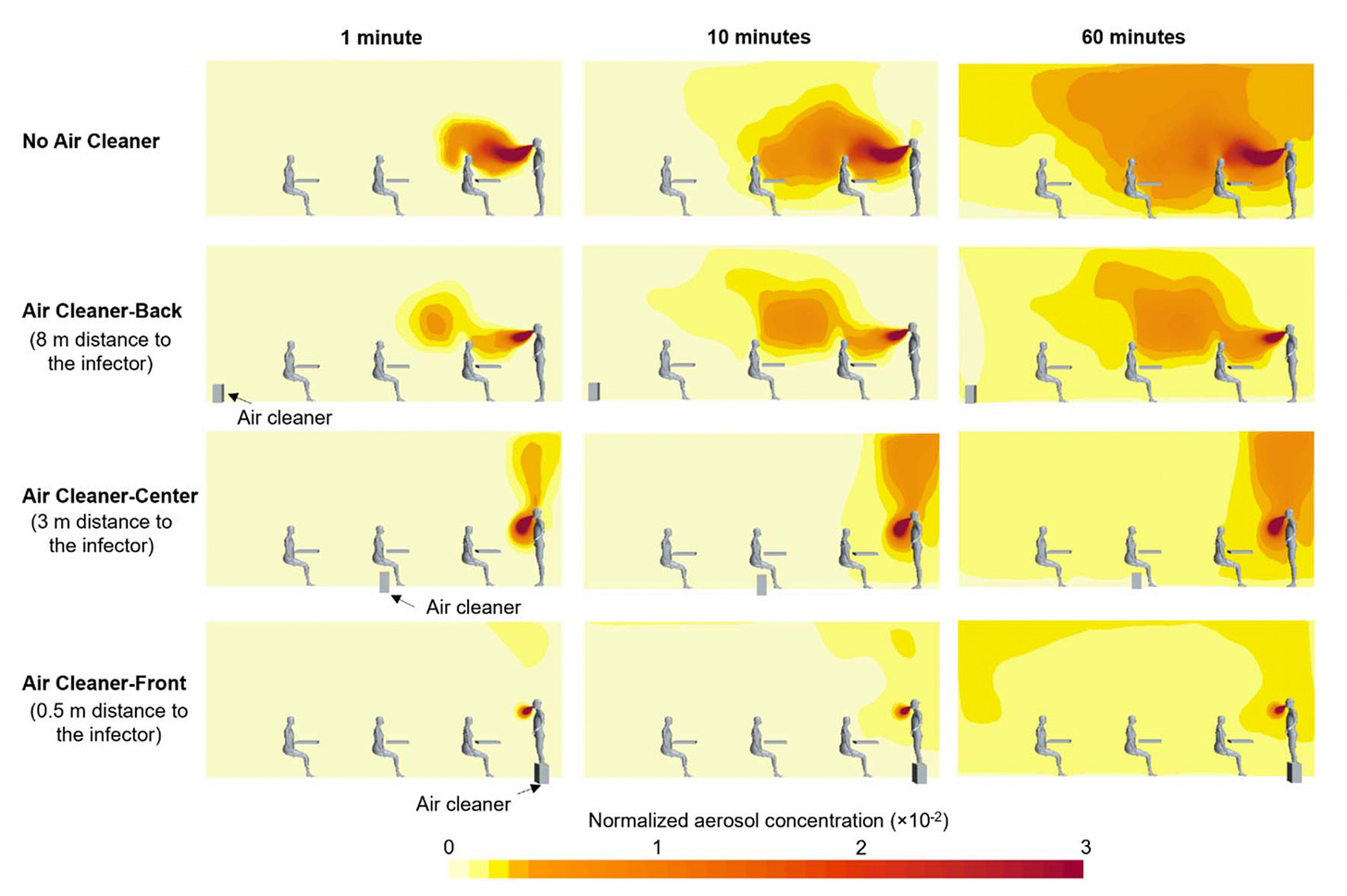
Let's throw out some of these portable air cleaners. You increase the air changes or clean air delivery pretty effectively for very low cost, and they work. And now the paper we just published in my team a couple of days ago starts to advance this more. We used a CFD model, so computational fluid dynamics. Essentially, you can look at the tracers and the airflow patterns in the room, and we learn a couple things that matter. Placement matters, so we like it in the center of the room if you can or as close as possible. And also the airflow matters. So the air cleaners are cleaning the air, but they're also moving the air, and that helps disperse these kind of clouds or plumes when an infected person is breathing or speaking. So you want to have good ventilation, good filtration. Also a lot of air movement in the space to help dilute and move around some of these respiratory particles so that they do get ventilated out or captured in a filter.
Eric Topol (00:24:40):
Yeah. So let me ask you, since we know outdoors are a lot safer. If you could do all these things indoors with filtration, air changing the quality, can you simulate the outdoors to get rid of the risk or markedly reduce the risk of respiratory viruses like SARS-CoV-2 and others?
Joseph Allen (00:25:04):
Yeah, you can't drop it to zero. There's no such thing as zero risk in any of these environments. But yeah, I think some of the estimates we've seen in my own team has produced in the 60-70% reduction range. I mean, if you do this right with really good ventilation filtration, you can drop that risk even further. Now, things like distancing matter, whether or not somebody's wearing a mask, these things are all going to play into it. But you can really dramatically drop the risk by handling just the basics of ventilation and filtration. And one way to think about it is this, distance to the infector still matters, right? So if you and I are speaking closely and I breathe on you, it's going to be hard to interrupt that flow. But you can reduce it through good ventilation filtration. But really what it's doing also is preventing super spreading events.
(00:25:55):
In other words, if I'm in the corner of a room and I'm infectious and you're on the other side, well if that room is sealed up pretty good, poor ventilation, no filtration, the respiratory aerosols are going to build up and your risk is going to increase and we're in there for an hour or two, like you would be in a room or office and you're exposed to infectious aerosol. With good ventilation filtration, those respiratory particles don't have a chance to reach you, or by the time they do, they're much further diluted. Linsey Marr I think was really great early in the pandemic by talking about this in terms of cigarette smoke. So a small room with no ventilation filtration, someone smoking in the corner, yeah, it's going to fill up over time with smoke you're breathing in that secondhand smoke. In a place with great ventilation filtration, that's going to be a lot further reduced, right? You're not going to get the buildup of the smoke and smoke particles are going to operate similarly to respiratory particles. So I think it's intuitive and it's logical. And if you follow public health guidance of harm reduction, risk reduction, if you drop exposure, you drop risk.
(00:26:58):
The goal is to reduce exposure. How do we do that? Well, we can modify the building which is going to play a key role in exposure reduction.
Eric Topol (00:27:06):
Now, to add to this, if I wear a sensor or have a sensor in the room for CO2, does that help to know that you're doing the right thing?
Joseph Allen (00:27:17):
Yeah, absolutely. So people who are not familiar with these air quality sensors. They're small portal air quality sensors. One of the things they commonly measure is carbon dioxide. We're the main source of CO2 inside. It's a really good indicator of ventilation rate and occupancy. And the idea is pretty simple. If the CO2 is low, you don't have a buildup of particles from the respiratory tract, right? And CO2 is a gas, but it's a good indicator of overall ventilation rate. This room I'm in right now at the Harvard School of Public Health has air quality sensors. We have this at Harvard Business School. We have it at the Harvard Health Clinics. Many other places are doing it, Boston Public schools have real-time air quality monitors. Here's the trick with CO2. So first I'll say we have some guidance on this at the Harvard Healthy Buildings page, if people want to go look it up, how to choose an air quality sensor, how to interpret CO2 levels.
Carbon Dioxide Levels
(00:28:04):
But here's a way to think about it. We generally would like to see CO2 levels less than 800 parts per million. Historically, people in my field have said under 1,000 is okay. We like to see that low. If your CO2 is low, the risk is low. If your CO2 is high, it doesn't necessarily mean your risk is high because that's where filtration can come in. So let me say that a little bit better. If CO2 is low, you're diluting enough of the respiratory particles. If it's high, that means your ventilation is low, but you might have excellent filtration happening. Either those MERV 13 filters we talked about or the portable air cleaners. Those filters don't capture CO2. So high CO2 just means you better have a good filter game in place or the risk is going to be high. So if you CO2 is low, you're in good shape. If it's high, you don't quite know. But if you have bad filtration, then the risk is going to be much higher.
Eric Topol (00:29:01):
I like that 800 number because that's a little lower than some of the other thresholds. And why don't we do as good as we can? The other question about is a particulate matter. So we are worried about the less than 5 microns, less than 2.5 microns. Can you tell us about that and is there a way that you can monitor that directly?
Joseph Allen (00:29:25):
Sure. A lot of these same sensors that measure CO2 also measure PM 2.5 which stands for particular matter. 2.5 microns is smaller, one of the key components of outdoor air pollution and EPA just set new standards, right? WHO has a standard for 5 microgram per cubic meter. EPA just lowered our national outdoor limit from 12 to 9 microgram per cubic meter. So that's a really good indicator of how well your filters are working. Here again, in a place like this or where you are, you should see particle levels really under 5 microgram per cubic meter without any major source happening. What's really interesting about those like the room I'm in now, when the wildfire smoke came through the East coast last year, levels were extraordinary outside 100, 200, 300 microgram per cubic meter. But because we have upgraded our filters, so we use MERV 15 here at Harvard, the indoor levels of particles stayed very low.
(00:30:16):
So it shows you how the power of these filters can actually, they do a really good job of capturing particles, whether it be from our lungs or from some other source. So you can measure this, but I'll tell you what's something interesting, if you want to tie it into our discussion about standards. So we think about particles. We have a lot of standards for outdoor air pollution. So there's a national ambient air quality standard 9 microgram per cubic meter. We don't have standards for indoor air quality. The only legally enforceable standard for indoor particles is OSHA's standard, and it's 5,000 microgram per cubic meter 5,000.
(00:30:59):
And it's absurd, right? It's an absurdity. Here we are EPAs, should it be 12, should it be 9, or should it be 8? And for indoors, the legally enforceable limit for OSHA 5,000. So it points to the big problem here. We talked about earlier about the need for these standards to codify some of this. Yes, we have awareness from the public. We have sensors to measure this. We have CDC now saying what we were saying with the Lancet COVID-19 Commission and elsewhere.
This is big movement, but the standards then need to come up behind it and get into code and new standards that are health focused and health based. And we have momentum, but we can't lose it right now because it's the first time in my career I felt like we're on the cusp of really getting this and we are so close. But of course it's always in danger of slipping through our fingers.
Regulatory Oversight for Air
Eric Topol (00:31:45):
Well, does this have anything to do with the fact that in the US there's no regulatory oversight over air as opposed to let's say Japan or other places?
Joseph Allen (00:31:57):
Yeah, I mean, we have regulatory oversight of outdoor air. That's EPA. There's a new bill that was introduced to give EPA more resources to deal with indoor air. EPA has got a great indoor air environments division, but it doesn't have the legally enforceable mandate or statute that we have for outdoor. So they'd give great guidance and have for a long time. I really like that group at EPA, but there's no teeth behind this. So what we have is worker health protections at OSHA to its own admission, says its standards are out of date. So we need an overhaul of how we think about the standards. I like the market driven approach. I think that's being effective, and I think we can do it from voluntary standards that can get adopted into code at the municipal level. I think that's a real path. I see it happening. I see the influence of all this work hitting legislators. So that's where I think the most promising path is for real change.
The Risks of Outdoor Air Pollution
Eric Topol (00:33:03):
Yeah, I think sidestepping, governmental teeth, that probably is going to be a lot quicker. Now, before we get to the cost issue, I do want to mention, as you know very well, the issue of air pollution in Science
a dedicated issue just a few weeks ago, it brought up, of course, that outdoor air pollution we've been talking about indoor is extraordinary risk for cancer, dementia, diabetes, I mean everything. Just everything. And there is an interaction between outdoor pollution and what goes on indoor. Can you explain basically reaffirm your concern about particulate matter outdoors, and then what about this interaction with what goes on indoors?
Joseph Allen (00:33:59):
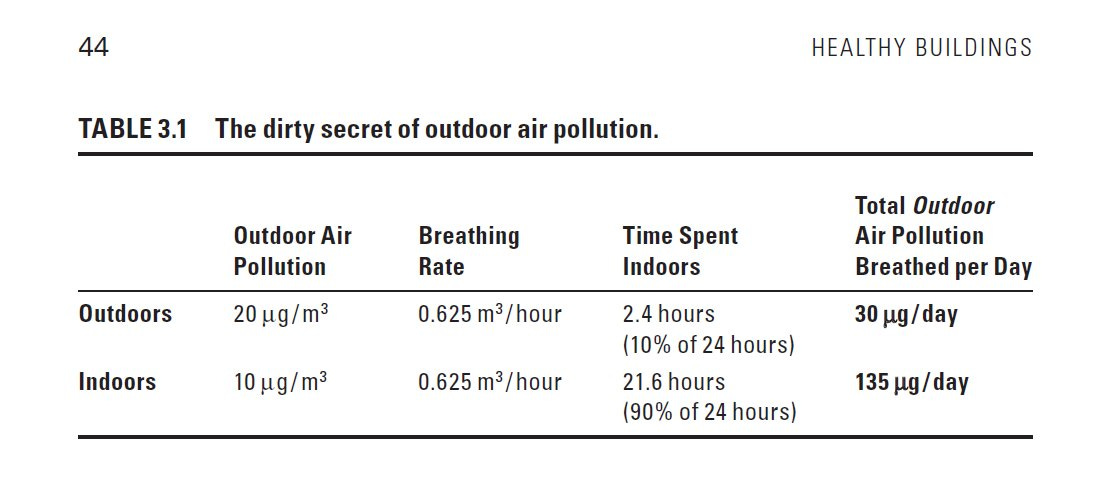
Yeah, so it's a great point. I mean, outdoor pollution has been one of the most studied environmental pollutants we know. And there's all of these links, new links between Alzheimer's, dementia, Parkinson's disease, anxiety, depression, cardiovascular health, you named it, right? I've been talking about this and very vocal. It's in the book and elsewhere I called the dirty secret of outdoor air pollution. The reality is outdoor air pollution penetrates indoors, and the amount depends on the building structure, the type of filters you have. But let's take an infiltration value of say 50%. So you have a lot of outdoor air pollution, maybe half of that penetrates inside, so it's lower, the concentration is lower, but 90% of the breaths you take are indoor. And if you do the math on it, it's really straightforward. The majority of outdoor air pollution you breathe happens inside.
(00:34:52):
And people, I think when they hear that think, wait, that can't be right. But that's the reality that outdoor pollution comes inside and we're taking so many breaths inside. Your total daily dose of outdoor air pollution is greater from the time you spend inside. I talk about this all the time. You see any article about outdoor air pollution, what's the cover picture? It's someone outside, maybe they're wearing a mask you can't really see. It's smoky hazy. But actually one of the biggest threats is what's happening inside. The nice thing here, again, the solutions are pretty simple and cost-effective. So again, upgrade from MERV 8 to MERV 13, a portable air cleaner. We are just capturing particles on a filter basic step that can really reduce the threat of outdoor air pollution inside. But it's ignored all the time. When the wildfire smoke hit New York City. New York City's orange, I called colleagues who are in the news business.
(00:35:48):
We have to be talking about the indoor threat because the guidance was good, but incomplete. Talk about Mayor Adams in New York City. Go inside, okay, that's good advice. And go to a place that has good filtration or they should have been giving out these low cost air cleaners. So just going inside isn't going to protect your lungs unless you're actually filtering a lot more of that air coming in. So trying to drive home the point here that actually we talk about these in silos. Well, wildfire smoke and particles, Covid and respiratory particles, we're all talking about these different environmental issues that harm our health, but they're all happening through or mediated by the building performance. And if we just get the building performance right, some basics around good ventilation, good filtration, you start to address multiple threats simultaneously. Outdoor air pollution, wildfire smoke, allergens, COVID-19, influenza, RSV, better cognitive function performance, anxiety. You start addressing the root cause or one of the contributors and buildings we can then start to leverage as a true public health tool. We have not taken advantage of the power of buildings to be a true public health tool.
Eric Topol (00:36:59):
Oh, you say it so well, and in fact your Table on page 44 in Healthy Buildings , we’ll link it because it shows quantitatively what you just described about outdoor and indoor cross fertilization if you will. Now before leaving air pollution outdoors, indoors, in order for us to affect this transformation that would markedly improve our health at the public health individual level, we're talking about a big investment. Can you put that in, you did already in some respects, but if we did this right in every school, I think in California, they're trying to mandate that in schools, in the White House, they're mandating federal buildings. This is just a little piece of what's needed. This would cost whatever trillions or hundreds of billions of dollars. What would it take to do this? Because obviously the health benefits would be so striking.
What’s It Gonna Cost?
Joseph Allen (00:38:04):
Well, I think one of the issues, so we can talk about the cost. A lot of the things I'm talking about are intentionally low cost, right? You look at the Lancet of COVID-19 Commission, our report we wrote a report on the first four healthy building strategies every building should pursue. Number one commission your building that's giving your building a tune-up. Well, guess what? That not only improves air quality, it saves energy and therefore saves money. It actually becomes cost neutral. If not provides an ROI after a couple of years. So that's simple. Increase the amount of outdoor air ventilation coming in that has an energy cost, we've written about this. Improved filtration, that's a couple bucks, really a couple bucks, this is small dollars or portable air cleaners, not that expensive. I think one of the big, and Lawrence Berkeley National Lab has written this famous paper people like to cite that shows there's $20 billion of benefits to the US economy if we do this.
(00:38:59):
And I think it points to one of the problems. And what I try to address in my book too, is that very often when we're having this conversation about what's it going to cost, we don't talk about the full cost benefit. In other words, we say, well, it's going to cost X amount. We can't do that. But we don't talk about what are the costs of sick buildings? What are the costs of kids being out of school for an entire year? What are the costs of hormonal disruption to an entire group of women in their reproductive years due to the material choices we make in our buildings? What are the costs to outdoor air pollution and cardiovascular disease, mental health? Because we don't have good filters in our buildings that cost a couple dollars. So in our book, we do this cost benefit analysis in the proforma in our book, we lay out what the costs are to a company. We calculate energy costs. We say these are the CapEx costs, capital costs for fixed costs and the OpEx costs for operating expenditures. That's a classic business analysis. But we factor in the public health benefits, productivity, reduced absenteeism. And you do that, and I don't care how you model it, you are going to get the same answer that the benefits far outweigh the cost by orders of magnitude.
Eric Topol (00:40:16):
Yeah, I want to emphasize orders of magnitude. Not ten hundred, whatever thousand X, right?
Joseph Allen (00:40:23):
What would be the benefit if we said we could reduce influenza transmission indoors in schools and offices by even a small percent because we improve ventilation and filtration? Think of the hospitalization costs, illness costs, out of work costs, out of school costs. The problem is we haven't always done that full analysis. So the conversation gets quickly to well, that's too much. We can't afford that. I always say healthy buildings are not expensive. Sick buildings are expensive. Totally leave human health out of that cost benefit equation. And then it warps this discussion until you bring human health benefits back in.
Forever Chemicals
Eric Topol (00:40:58):
Well, I couldn't agree more with you and I wanted to frame this by giving this crazy numbers that people think it's going to cost to the reality. I mean, if there ever was an investment for good, this is the one that you've outlined so well. Alright, now I want to turn to this other topic that you have been working on for years long before it kind of came to the fore, and that is forever chemicals. Now, forever chemicals, I had no idea that back in 2018 you coined this term. You coined the term, which is now a forever on forever chemicals. And basically, this is a per- and polyfluoroalkyl substances (PFAS), but no one will remember that. They will remember forever chemicals. So can you tell us about this? Because this of course recently, as you know well in May in the New Yorker, there was an expose of 3M, perhaps the chief offender of these. They're everywhere, but especially they were in 3M products and continue to be in 3M products. Obviously they've been linked with all kinds of bad things. What's the story on forever chemicals?
Joseph Allen (00:42:14):
Yeah, they are a class of chemicals that have been used for decades since the forties. And as consumers, we like them, right? They're the things that make your raincoat repel rain. It makes your non-stick pan, your scrambled eggs don't stick to the pan. We put them on carpets for stain resistance, but they came with a real dark side. These per- and polyfluoroalkyl substances, as I say, a name only a chemist could love have been linked with things like testicular cancer, kidney cancer, interference with lipid metabolism, other hormonal disruption. And they are now a global pollutant. And one of the reasons I wrote the piece to brand them as forever chemicals was because I'm in the field of environmental health. We had been talking about these for a long time and I just didn't hear the public aware or didn't capture their attention. And part of it, I think is how we talk about some of these things.
(00:43:14):
I think a lot about this. Per- and polyfluoroalkyl substances, no one's going to, so the forever chemicals is actually a play on their defining feature. So these chemicals, these stain repellent chemicals are characterized by long chains of the carbon fluorine bond. And when we string these together that imparts this and you put them on top of a product that imparts the property of stain resistance, grease resistance, water resistance, but the carbon fluorine bond is the strongest in all of organic chemistry. And these chains of the carbon fluorine bond never fully break down in the environment. And when we talk in my field about persistent organic pollutants, we talk about chemicals that break down on the order of decades. Forever chemicals don't break down. They break down the order of millennia. That's why we're finding them everywhere. We know they're toxic at very low levels. So the idea of talking about forever chemicals, I wanted to talk about their foreverness.
(00:44:13):
This is permanent. What we're creating and the F and the C are the play on the carbon-fluorine bond and I wrote an article trying to raise awareness about this because some companies that have produced these have known about their toxicity for decades, and it's just starting the past couple of years, we're just starting to pay attention to the scale of environmental pollution. Tens of millions of Americans have forever chemicals in their drinking water above the safe limit, tens of millions. I worked as an expert in a big lawsuit for the plaintiffs that were drinking forever chemicals in their water that was dumped into the drinking water supply by a manufacturing company. I met young men with testicular cancer from drinking forever chemicals in their water. These really has escaped the public's consciousness, it wasn't really talked about. Now of course, we know every water body, we use these things in firefighting foams or every airport has water pollution.
(00:45:17):
Most airports do. Firefighters are really concerned about this, high rates of cancer in the firefighter population. So this is a major problem, and the cleanup is not straightforward or easy because they're now a global pollutant. They persist forever. They're hard to remediate and we're stuck with them. So that's the downside, I can talk about the positives. I try to remain an optimist or things we're doing to try to solve this problem, but that's ultimately the story. And my motivation was I just to have people have language to be able to talk about this that didn't require a degree in organic chemistry to understand what they were.
Eric Topol (00:45:52):
Yeah, I mean their pervasiveness is pretty scary. And I am pretty worried about the fact that we still don't know a lot of what they're doing in terms of clinical sequela. I mean, you mentioned a couple types of cancer, but I don't even know if there is a safe threshold.
Joseph Allen (00:46:16):
Eric, I'll tell you one that'll be really interesting for you. A colleague of mine did a famous study on forever chemicals many years ago now and found that kids with higher levels of forever chemicals had reduced vaccine effectiveness related to these chemicals. So your point is, right, a lot of times we're using these industrial chemicals. We know a couple endpoints for their affecting our bodies, but we don't know all of them. And what we know is certainly alarming enough that we know enough to know we shouldn't be using them.
Eric Topol (00:46:51):
And you wrote another masterful op-ed in the Washington Post, 6 forever chemical just 10,000 to go. Maybe you could just review what that was about.
Joseph Allen (00:47:02):
Yeah, I've been talking a lot about this issue I call chemical whack-a-mole. So forever chemical is the perfect example of it. So we finally got people's attention on forever chemicals. EPA just regulated 6 of them. Well, guess what? There are 10,000 if not many more than that. Different variants or what we call chemical cousins. Now that's important for this reason. If you think about how we approach these from a regulatory standpoint, each of the 10,000 plus forever chemicals are treated as different. So by the time EPA regulates 6, that's important. It does free up funding for cleanup and things like this. But already the market had shifted away from those 6. So in other words, in the many thousand products that still use forever chemicals, they're no longer using those 6 because scientists have told people these things are toxic years ago. So they switch one little thing in the chemical, it becomes a new chemical from a regulatory perspective.
(00:47:57):
But to our bodies, it's the same thing. This happens over and over. This has happened with pesticides. It happens with chemicals and nail polish. It happens in chemicals in e-cigarettes. It happens with flame retardant chemicals. I wrote a piece in the Post maybe six years ago talking about chemical whack-a-mole, and this problem that we keep addressing, these one-off, we hit one, it changes just slightly. Chemical cousin pops up, we hit that one. Five years later, scientists say, hey, the next one doesn't look good either. We're doing this for decades. It's really silly. It's ineffective, it's broken, and there are better ways to handle this going forward.
Eric Topol (00:48:31):
And you know what gets me, and it's like in the pharma industry that I've seen the people who run these companies like 3M that was involved in a multi-decade coverup, they're never held accountable. I mean, they know what they're doing and they just play these games that you outlined. They're still using 16,000 products, according to the New Yorker, the employee that exposed them, the whistleblower in the New Yorker article.
Joseph Allen (00:48:58):
That was an amazing article by Sharon Lerner talking to the people who had worked there and she uncovered that they knew the toxicity back in the seventies, and yes, they were still making these products. One of the things that I think has gotten attention of some companies is while the regulations have been behind, the lawsuits are piling up.
Joseph Allen (00:49:21):
The lawsuit I was a part of as an expert for that was about an $800 million settlement in favor of the plaintiffs. A couple months later is another one that was $750 million. So right there, $1.5 billion, there's been several billion dollars. This has caught the attention of companies. This has caught the attention of product manufacturers who are using the forever chemicals, starting to realize they need to reformulate. And so, in a good way now, that's not the way we should be dealing with this, but it has started to get companies to wake up that maybe they had been sleeping on it, that this is a major problem and actually the markets have responded to it.
Eric Topol (00:50:02):
Well, that's good.
Joseph Allen (00:50:03):
Because these are major liabilities on the books.
Eric Topol (00:50:05):
Yeah, I mean, I think what I've seen of course with being the tobacco industry and I was involved with Vioxx of course, is the companies just appeal and appeal and it sounds really good that they've had to pay $800 million, but they never wind up paying anything because they basically just use their muscle and their resources to appeal and put it off forever. So I mean, it's one way to deal with it is a litigation, but it seems like that's not going to be enough to really get this overhauled. I don't know. You may be more sanguine.
Joseph Allen (00:50:44):
No, no, I agree with you. It's the wrong way. I mean, we don't want to, the solution here is not to go after companies after people are sick. We need get in front of this and be proactive. I mentioned it only because I know it has made other companies pay attention how many billion does so-and-so sue for. So that's a good signal that other companies are starting to move away from forever chemicals. But I do want to talk about one of the positive approaches we're doing at Harvard, and we have a lot of other partners in the private sector doing this. We're trying to turn off the spigot of forever chemicals entering the market in the first place. As a faculty advisor to what we call the Harvard Healthier Building Materials Academy, we publish new standards. We no longer buy products that have forever chemicals in them for our spaces.
(00:51:31):
So we buy a chair or carpet. We demand no forever chemicals. What's really neat about this is we also say, we treat them as a whole class. We don't say we don't want PFOA. That's one of the regulated chemicals. We say we don't want any of the 10,000. We are not waiting for the studies to show us they act like the other ones. We've kind of been burned by this for decades. So we're actually telling the suppliers we don't want these chemicals and they're delivering products to us without these chemicals in them. We have 50 projects on our campus built with these new design standards without forever chemicals and other toxic chemicals. We've also done studies that a doctoral student done the study. When we do this, we find lower levels of these chemicals in air and dust, of course. So we're showing that it works.
(00:52:19):
Now, the goal is not to say, hey, we just want to make Harvard a healthier campus and the hell with everybody else. The goal is to show it can be done with no impact to cost, schedule or product performance. We get a healthier environment, products look great, they perform great. We've also now partnered with other big companies in the tech industry in particular to try and grow or influence the market by saying, look how many X amount of purchasing dollars each year? And it's a lot, and we're demanding that our carpets don't have this, that our chairs don't have it, and the supply chain is responding. The goal, of course, is to just make it be the case that we just have healthy materials in the supply chain for everybody. So if you or I, or anybody else goes to buy a chair, it just doesn't have toxic chemicals in it.
Eric Topol (00:53:06):
Right, but these days the public awareness still isn't there, nor are the retailers that are selling whether it's going to buy a rug or a chair or new pots and pans. You can't go in and say, does this have any forever chemicals? They don't even know, right?
Joseph Allen (00:53:24):
Impossible. I study this and it's hard for me when I go out to try and find and make better decisions for myself. This is one of the reasons why we're working, of course, trying to help with the regulatory side, but also trying to change the market. Say, look, you can produce the similar product without these chemicals, save yourself for future lawsuits. Also, there's a market for healthy materials, and we want everybody to be a part of that market and just fundamentally change the supply chain. It's not ideal, but it's what we can do to influence the market. And honestly, we're having a lot of impact. I've been to these manufacturing plants where they have phased out these toxic chemicals.
Eric Topol (00:54:03):
That’s great to hear.
Joseph Allen (00:54:06):
And we see it working on our campus and other companies’ campuses.
Eric Topol (00:54:10):
Well, nobody can ever accuse you of not taking on big projects, okay.
Joseph Allen (00:54:15):
You don't get into public health unless you want to tackle the big ones that are really going to influence.
Micro(nano) Plastics
Eric Topol (00:54:20):
Well, that's true, Joe, but I don't know anybody who's spearheading things like you. So it's phenomenal. Now before we wrap up, there's another major environmental problem which has come to the fore, which are plastics, microplastics, nanoplastics. They're everywhere too, and they're incriminated with all the things that we've been talking about as well. What is your view about that?
Joseph Allen (00:54:48):
Well, I think it's one, well, you see the extent of the pollution. It's a global pollutant. These are petrochemicals. So it's building up, and these are fossil fuel derivatives. So you can link this not just to the direct human health impacts, the ecosystem impacts, but also ecosystem and health impacts through climate change. So we've seen our reliance on plastics grow exponentially over the past several decades, and now we're seeing the price we're paying for that, where we're seeing plastics, but also microplastics kind of everywhere, much like the forever chemicals. Everywhere we look, we find them and we're just starting to scratch a surface on what we know about the environmental impacts. I think there's a lot more that can be done here. Try to be optimistic again, at least if you find a problem, you got to try and point to some kind of solution or at least a pathway towards solutions.
(00:55:41):
But I like some of the stuff from others colleagues at Yale in particular on the principles of green chemistry. I write about them in my book a little bit, but it's this designing for non-permanence or biodegradable materials so that if we're using anything that we're not leaving these permanent and lasting impacts on our ecosystem that then build up and they build up in the environment, then they build up in all of us and in our food systems. So it seems to me that should be part of it. So think about forever chemicals. Should we be using chemicals that never break down in the environment that we know are toxic? How do we do that? As Harvard, one of the motivating things here for forever chemicals too, is how are we ignoring our own science? Everyone's producing this science, but how do we ignore even our own and we feel we have responsibility to the communities next to us and the communities around the world. We're taking action on climate change. How are we not taking action on these chemicals? I put plastics right in there in terms of the environmental pollutants that largely come from our built environment, food products and the products we purchase and use in our homes and in our bodies and in all the materials we use.
Eric Topol (00:56:50):
When you see the plastic show up in our arteries with a three, four-fold increase of heart attacks and strokes, when you see it in our testicles and every other organ in the body, you start to wonder, are we ever going to do something about this plastic crisis? Which is somewhat distinct from the forever chemicals. I mean, this is another dimension of the problem. And tying a lot of this together, you mentioned, we are not going to get into it today, but our climate crisis isn't being addressed fast enough and it's making all these things exacerbating.
Joseph Allen (00:57:27):
Yeah, let me touch on that because I think it is important. It gets to something I said earlier about a lot of these problems we treat as silos, but I think a lot of the problems run through our buildings, and that means buildings are part of the solution set. Buildings consume 40% of global energy.
(00:57:42):
Concrete and steel count for huge percentages of our global CO2 emissions. So if we're going to get climate solved, we're going to have to solve it through our buildings too. So when you start putting this all together, Eric, right, and this is why I talk about buildings as healthy buildings could potentially be one of the greatest public health interventions we have of this century. If we get it right, and I don't mean we get the Covid part, right. We get the forever chemicals part, right. Or the microplastics part, right. If you start getting this all right, good ventilation, better filtration, healthy materials across the board, energy efficient systems, so we're not drawing on the energy demand of our buildings that are contributing to the climate crisis. Buildings that also address climate adaptation and resilience. So they protect us from extreme heat, wildfire smoke, flooding that we know is coming and happening right now.
(00:58:37):
You put that all together and it shows the centrality of buildings on our collective health from our time spent indoors, but also their contribution to environmental health, which is ultimately our collective human health as well. And this is why I'm passionate about healthy buildings as a real good lens to put this all under. If we start getting these right, the decisions we make around our buildings, we can really improve the human condition across all of these dimensions we're talking about. And I actually don't think it's all that hard in all of these. I've seen solutions.
Eric Topol (00:59:12):
I'm with you. I mean, there's innovations that are happening to take the place of concrete, right?
Joseph Allen (00:59:20):
Sure. We have low emission concrete right now that's available. We have energy recovery ventilation available right now. We have real time sensors. We can do demand control ventilation right now. We have better filters right now. We have healthy materials right now.
(00:59:33):
We have this, we have it. And it's not expensive if we quantify the health benefits, the many, many multiple benefits. So it's all within our reach, and it's just about finding these different pathways. Some of its market driven, some of it's regulatory, some of it's at the local level, some of it's about raising awareness, giving people the language to talk about these things. So I do think it's the real beginning of the healthy buildings era. I really, truly believe it. I've never seen change like this in my field. I've been chasing sick buildings for a long time.
Joseph Allen (01:00:11):
And clearly there's pathways to do better.
Eric Topol (01:00:13):
You're a phenom. I mean, really, you not only have all the wisdom, but you articulate it so well. I mean, you’re leading the charge on this, and we're really indebted to you. I'm really grateful for you taking an hour of your busy time to enlighten us on this. I think what you're doing is it's going to keep you busy for your whole career.
Joseph Allen (01:00:44):
Well, the goal here is for me to put myself out of business. We shouldn't have a healthy buildings program. It just should be the way it's done. So I'm looking forward to the time out of business, hopefully have a healthy building future, then I can retire, be happy, and we'll be onto the next big problem.
Eric Topol (01:00:57):
We'll all be following your writings, which are many, and fortunately not just for science publications, but also for the public though, they're so important because the awareness level as I can't emphasize enough, it's just not there yet. And I think this episode is going to help bring that to a higher level. So Joe, thank you so much for everything you're doing.
Joseph Allen (01:01:20):
Well, I appreciate it. Thanks for what you're doing too, and thanks for inviting me on. We can't get the word out unless we start sharing it across our different audiences, so I appreciate it. Thanks so much.
Eric Topol (01:01:28):
You bet.
***********************************************
A Poll
Thanks for listening, reading or watching!
The Ground Truths newsletters and podcasts are all free, open-access, without ads.
Please share this post/podcast with your friends and network if you found it informative!Voluntary paid subscriptions all go to support Scripps Research. Many thanks for that—they greatly helped fund our summer internship programs for 2023 and 2024.
Thanks to my producer Jessica Nguyen and Sinjun Balabanoff for audio and video support at Scripps Research.
Note: you can select preferences to receive emails about newsletters, podcasts, or all I don’t want to bother you with an email for content that you’re not interested in.



















Share this post